2. Department of Neurosurgery, Tsinghua University Yuquan Hospital, Beijing 100040, China
Objective: To review and discuss the etiology, diagnosis and treatment C3 of bilateral cervical spondylolysis.
Methods: This was a retrospective review of the clinical features, imaginge findings, and treatment of 4 cases of bilateral C3 cervical spondylolysis, with a review of the literature.
Results: A 21-year-old woman, a 26-year-old man, a 14-year-old boy, and a 46-year-old man were diagnosed with bilateral C3 cervical spondylolysis. The patients had characteristic bilateral clefts between the articular pillar and the facets of C3, as well as spina bifida on CT. Although spondylolisthesis was not observed, spinal cord compression was definitive. All patients underwent posterior decompression with satisfactory results.
Conclusions: C3 cervical spondylolysis is rare condition. The cause is most likely congenital. Diagnosis is dependent on characteristic radiological features. Surgical treatment is the first choice.
1 Introduction Cervical spondylolysis is a relatively rare anomaly, with only about 100 cases described worldwide[1]. It is defined as a corticated cleft between the superior and inferior articular facets of the articular pillar,and is considered the cervical equivalent of the pars interarticularis in the lumbar spine[2]. The anomaly is most commonly seen at C6,followed by C4,and rarely reported to involve C3. To our knowledge,the anomaly has been reported in only one Chinese patient with C6 spondylolysis[3]. We report the clinical and radiological findings in 4 Chinese patients diagnosed with C3 cervical spondylolysis and managed in our hospital. These reports are presented along with the current literature on cervical spondylolysis,with a focus on clinical diagnosis,treatment,and follow-up.
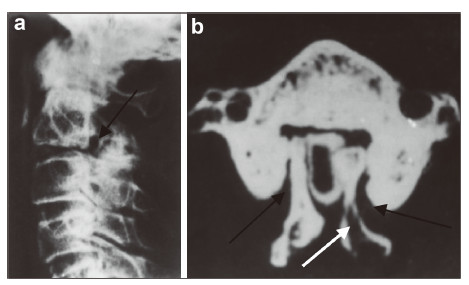
2 Case reports 2.1 Case 1 A 21‐year‐old woman sustained an extension injury in a traffic accident 1 month before admission. Physical examination revealed a limited range of neck motion due to posterior neck pain. The neurologic examination was normal. Palpation of her neck revealed severe tenderness in the upper cervical spine. Lateral view plain radiography identified a hypoplastic articular mass at C3 (Figure 1). Iodine contrast revealed a narrowed spinal canal at C3 on computed tomography (CT). The lateral mass at C3 was discontinuous and typical features of spina bifida were revealed. The surfaces of the spondylolysis were smooth,suggesting a chronic process. Spinal cord compression was definitive,while spondylolisthesis was not observed. The compression was located mainly at the posterior column and instability was not present; posterior decompression was performed,and the symptoms were relieved after surgery.
|
| Figure 1 A 21‐year‐old woman presented with bilateral C3 spondylolysis.(a) Lateral view plain radiography showing a cleft of the articular pillar,with a bow‐tie configuration (black arrow). (b) On CT,the lateral mass at C3 was discontinuous,with a typical features of spina bifida (white arrow),and was well‐corticated (black arrow). |
|
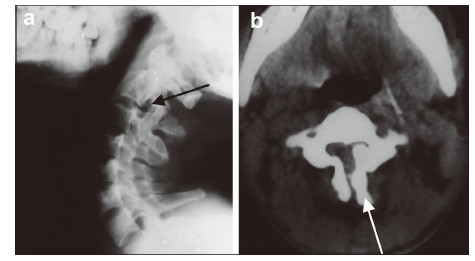
| Figure 2 A 26‐year‐old man presented with bilateral C3 spondylolysis. (a) Lateral view plain radiography showing a hypoplastic articular mass and spinal process at C2(black arrow).(b) Iodine contrast CT showing bilateral clefts between the articular pillar and the facets of C3 as well as spina bifida (white arrow). |
|
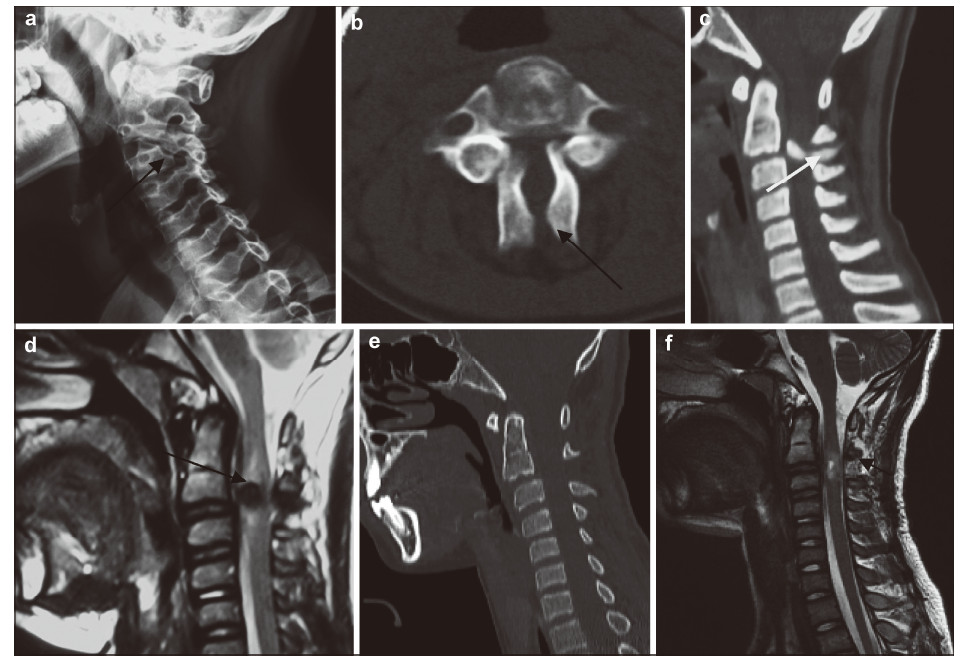
| Figure 3 A 14‐year‐old boy presented with bilateral C3 spondylolysis.(a) Oblique view plain radiography showing a cleft of the articular pillar (arrow).(b) On axial CT,the lateral mass at C3 was discontinuous,with typical features of spina bifida (arrow).(c,d) A bony density (white arrow) and low cord signal (black arrow) change was observed at the spondylolytic level.(e,f) Follow‐up CT showed the bony density had disappeared and MRI showed a slightly high cord signal (arrow). |
|
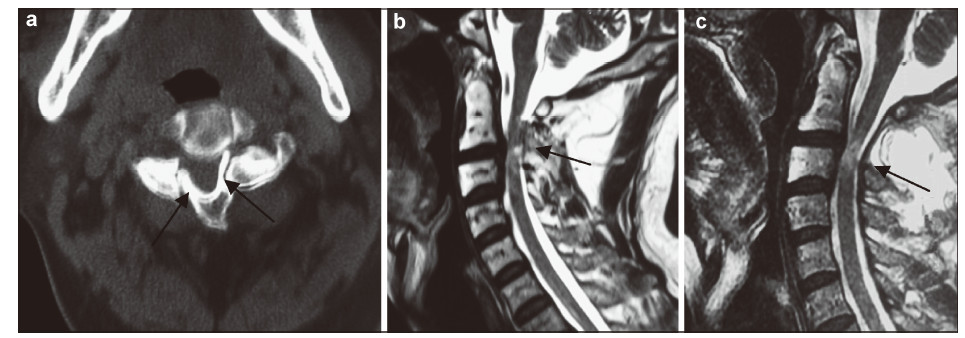
| Figure 4 A 45-year-old man presented with bilateral C3 spondylolysis.(a) Axial CT scan revealed well‐corticated clefts between the bilateral C3 facets (arrows).(b) On sagittial MRI,the canal at the spondylolytic level was narrow and the subarachnoid space disappeared (arrow).(c) Follow‐up MRI showed the subarachnoid space was clear (arrow). |
This condition is rare,and the exact cause of cervical spondylolysis remains unknown. Schwartz et al.[11] suggested that cervical spondylolysis is caused by posttraumatic nonunion with pseudarthrosis. Morvan et al. and Cautilli et al.[12, 13] believed that cervical spondylolysis arises from repetitive microtrauma resulting in stress fractures to the pars region,which is similar to the process causing lumbar spondylolysis. They also pointed out that spondylolysis has not been reported in an infant and that the transitional vertebra (C6) is the most common level,lending further support for their microtrauma theory. However,many patients do not present with a significant history of trauma. Only one of our patients had a history of acute neck injury. In other reports,the anomaly showed wellcorticated margins,without evidence of fresh fracture on MRI or CT[9, 14]. Moreover,our 4 cases were all diagnosed with bilateral C3 cervical spondylolysis. Hence,many authors contend that congenital or faulty ossification within the single ossification center of the articular mass is the etiology of cervical spondylolysis[11, 15, 16, 17]. Based on observations in our cases,we support congenital theories.
Clinically,the symptoms of cervical spondylolysis vary,ranging from neck stiffness,rigidity,nuchal pain with or without radicular symptoms,and bladder dysfunction. Some authors reported that over 70% of the cases were seen at hospitals because of neck pain with or without injuries[18]. In this report,2 of the 4 cases had bladder and bowel dysfunction. Some cases are asymptomatic. The diagnosis of cervical spondylolysis mainly depends on the characteristic radiological features. Cervical spondylolysis has characteristic imaging findings. Vertical spondylolytic clefts were present between the superior and inferior facets of the articular pillar of the cervical spine,each of which had a smooth cortical border. Forsberg et al. reported a characteristic “cleft bow tie” or “bat wing” in the sagittal plain[15]. In addition,three‐dimensional reconstructed CT of the cervical spine showed a triangular shape of the pillar fragments,divided by a cleft[3]. The presence of these characteristic features on plain films or CT can provide a definitive diagnosis. MRI often cannot identify a spondylolytic defect, with absence of visualization of the spinous process anomaly on sagittal sequences. However,MRI plays an important role in evaluating the spinal cord. Clinically,it is important to differentiate cervical spondylolysis from acute laminal fractures. Acute cervical spine injuries present with low signal change and cord atrophy on T2WI MRI. In our report,the 4 cases were diagnosed with bilateral C3 cervical spondylolysis. They had characteristic bilateral clefts between the articular pillar and the facets of C3,as well as spina bifida on CT.
Operative and nonoperative treatment is reported in the literature. Poggi et al. and Goupille et al. all contended that surgical intervention should be considered when nonoperative therapy fails or when symptoms are present indicating an unstable spondylolytic defect[9, 19]. Ahn et al. concluded that surgical treatment should be the first choice for cases where there is instability of the lamina[10]. The same study also reported that anterior interbody fusions were performed during surgical treatment. In our cases, the articular defect protruded into the spinal canal and caused cord compression. Hence,all patients underwent surgery. The compression was located mainly at the posterior column and instability was not present. However,C3 is not the transitional vertebra and is subjected to stress less often. Therefore,posterior decompression was performed,and the symptoms were relieved after surgery.
In conclusion,C3 cervical spondylolysis is rare. The exact cause remains controversial and most likely is congenital in origin. Its diagnosis is dependent on characteristic radiological features. It is important to differentiate from acute cervical spine injuries. Surgical treatment is the first choice for cases where there is compression of the spinal cord or instability of the lamina.
Conflict of interests The authors have no financial interest to disclose regarding the article.| [1] | Amin MF, Mollano AV, Weinstein SL, El-Khoury GY. Rare bilateral C6 spondylolysis and spondylolisthesis in an adolescent athlete:Evaluation with magnetic resonance imaging and multidetector computerized tomography. Spine , 2006, 31(21):E823-E825. |
| Click to display the text | |
| [2] | Legaye J, Horduna M. Cervical spondylolysis in a child:A case with hypermobility. Spine J , 2009, 9(1):E15-E19. |
| Click to display the text | |
| [3] | Tam ACW, Leung JLY, Lau KY, Yee PK. Bilateral cervical spondylolysis in a young Chinese woman presenting with a neck injury. Hong Kong Med J , 2008, 14(4):324-326. |
| Click to display the text | |
| [4] | Hadley LA. Congenital absence of pedicle from the cervical vertebra. Am J Roentgenol Radium Ther , 1946, 55(4):193-197. |
| Click to display the text | |
| [5] | Perlman R, Hawes LE. Cervical spondylolisthesis. J Bone Joint Surg Am , 1951, 33(4):1012-1013. |
| Click to display the text | |
| [6] | Sasa T, Yoshizumi Y, Imada K, Aoki M, Terai T, Koizumi T, Goel VK, Faizan A, Biyani A, Sakai T, Sairyo K. Cervical spondylolysis in a judo player:A case report and biomechanical analysis. Arch Orthop Trauma Surg , 2009, 129(4):559-567. |
| Click to display the text | |
| [7] | Schwartz JM. Case 36:Bilateral cervical spondylolysis of C6. Radiology , 2001, 220(1):191-194. |
| Click to display the text | |
| [8] | McAnany S, Cho S, Qureshi S, Hecht AC. A commentary on cervical spondylolysis in the contact athlete. Spine J , 2014, 14(6):e7-e8. |
| Click to display the text | |
| [9] | Poggi JJ, Martinez S, Hardaker WT Jr, Richardson WJ. Cervical spondylolysis. J Spinal Disord , 1992, 5(3):349-356. |
| Click to display the text | |
| [10] | Ahn PG, Yoon DH, Shin HC, Kim KN, Yi S, Lee DY, Yang MS, Ha Y. Cervical spondylolysis. Spine , 2010, 35(3):e80-e83. |
| Click to display the text | |
| [11] | Schwartz AM, Wechsler RJ, Landy MD, Wetzner SM, Goldstein SA. Posterior arch defects of the cervical spine. Skeletal Radiol , 1982, 8(2):135-139. |
| Click to display the text | |
| [12] | Morvan G, Busson J, Frot B, Nahum H. Cervical spondylolysis. 7 cases. Review of the literature. J Radiol , 1984, 65(4):259-266. (in French) |
| Click to display the text | |
| [13] | Cautilli RA, Joyce MF, Lin PM. Congenital elongation of the pedicles of the sixth cervical vertebra in identical twins. J Bone Joint Surg Am , 1972, 54(3):653-656. |
| Click to display the text | |
| [14] | Nishimura Y, Ellis MJ, Anderson J, Hara M, Natsume A, Ginsberg HJ. Progressively unstable C2 spondylolysis requiring spinal fusion:Case report. Neurol Med Chir (Tokyo) , 2014, 54(9):761-767. |
| Click to display the text | |
| [15] | Forsberg DA, Martinez S, Vogler JB 3rd, Wiener MD. Cervical spondylolysis:Imaging findings in 12 patients. Am J Roentgenol , 1990, 154(4):751-755. |
| Click to display the text | |
| [16] | Buchholz AL, Morgan SL, Robinson LC, Frankel BM. Minimally invasive percutaneous screw fixation of traumatic spondylolisthesis of the axis. J Neurosurg Spine , 2015, 22(5):459-465. |
| Click to display the text | |
| [17] | Domenicucci M, Pescatori L, Marruzzo D, Colistra D, Missori P. Cervical congenital spondylolytic spondylolisthesis associated with duplication of the vertebral artery:Case report. Spine J , 2014, 14(9):e1-e5. |
| Click to display the text | |
| [18] | Hirota S, Amano K, Maeno T, Doi T. A case of cervical spondylolysis causing tetraplegia. Spine , 1988, 13(1):113-116. |
| Click to display the text | |
| [19] | Goupille P, Fouquet B, Cotty P, Valat JP. Cervical spondylolysis. Am J Roentgenol , 1991, 157(5):1127-1128. |
| Click to display the text |



