Malignant transformation and treatment of cystic mixed germ cell tumor
1 Case presentation
1.1 History
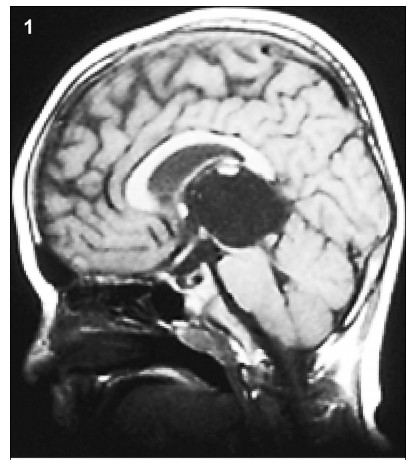
A space-occupied cystic lesion in the rear of the third
ventricle was detected in an 8-year-old boy presenting with symptoms of raised intracranial pressure
(ICP) and a diagnosis of “cystic lesion” 3 years
ago (
Figure 1). He underwent a ventricle-peritoneal
shunt operation without serum tumor marker test
and became asymptomatic soon after the operation.
Intermittent regular brain Magnetic Resonance
Imaging (MRI) demonstrated no evidence of massive
aggrandizement during the following 2 years. Then,
2 months ago,he rapidly developed unsteady gait
and confined ocular motor function,followed by acute
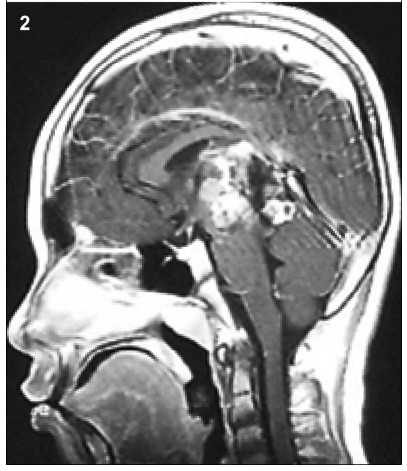
aggravating clinical symptoms. MRI scans showed
that the mass had remarkably enlarged in size and the
solid component had become predominant,instead of
the prior cystic lesion. Furthermore,the transitional
parenchyma tumor was heterogeneously and notably
enhanced in contrast-enhanced MR image (
Figure 2).
1.2 Admission conditions
As a result of the large tumor compressing the midbrain,the boy was somnolent,unable to walk,and
had jerking and increased muscle tension in all four
limbs. Neurological examination revealed left ptosis,
anisocoria (left 3 mm; right 2.5 mm),bilateral sluggish
pupillary light reflex,restricted eyeball abduction,and
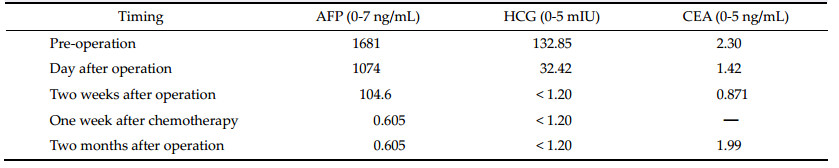
bilateral Parinaud Syndrome. Serum tumor marker
level investigation showed remarkably raised serum
Alpha 1-fetoprotein (AFP) and human chorionic
gonadotropin (HCG ),but carcino-embryonic antigen
(CEA) was normal (
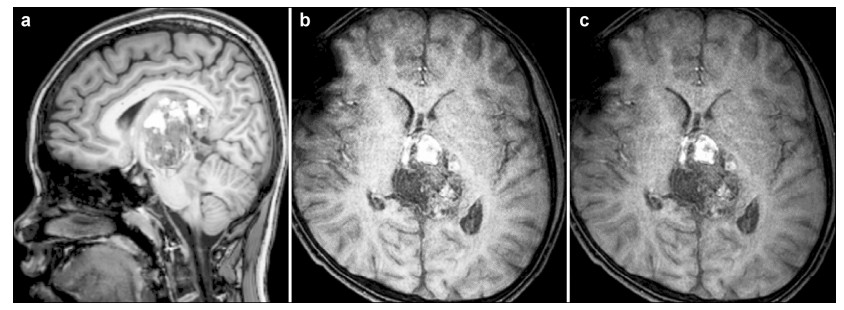
Table 1). Brain MR scans (T1 and
SWIp) illustrated enhanced heterogeneous signal and
hemorrhagic appearance of the mass (
Figures 3a and
3b). Another specific MR (SWIp sequence) scan showed
simple blood supply signal on the backside of the tumor capsule (
Figure 3c). Diffusion-tensor MR imaging
(DTI) described an integrated framework of the corpus
callosum and cerebral fornix (
Figure 4).
Table 1 Preoperative and postoperative serum tumor marker levels
1.3 Treatment procedure
The patient underwent frontal lobe and longitudinal
craniotomy via a transcallosal-interforniceal approach.
The elongated thalamic intermediate block could be
seen. The tumor was noted to have various heterogeneous components,as well as remote hemorrhage
with integrated tumor capsule,and was completely
removed piece by piece. The patient had a seemingly
satisfactory subsequent recovery,except for slight
oculomotor abnormality and short-term memory
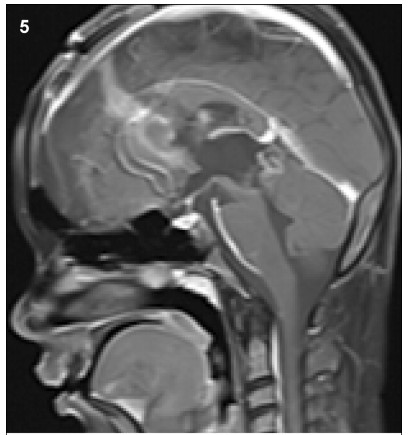
dysfunction relieved within 2 weeks. Postoperative
CT scan and MR imaging revealed total resection
of the mass (
Figure 5). Adjuvant cisplatin-based
chemotherapy (5 days per cycle) was commenced at
the 2
nd week after operation. The patient’s serum
tumor marker level declined to normal 1 week after
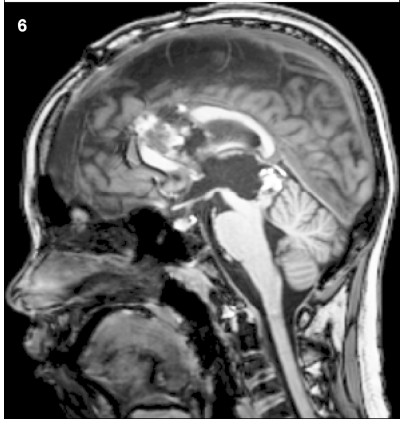
chemotherapy,and synchronous MR imaging showed
little hemorrhagic necrotic signal (
Figure 6). Diffusiontensor imaging described partial destruction of
the nerve fasciculus along the corpus callosum and
integrated framework of the left fornix (
Figure 7).
The patient returned to school as usual 2 months
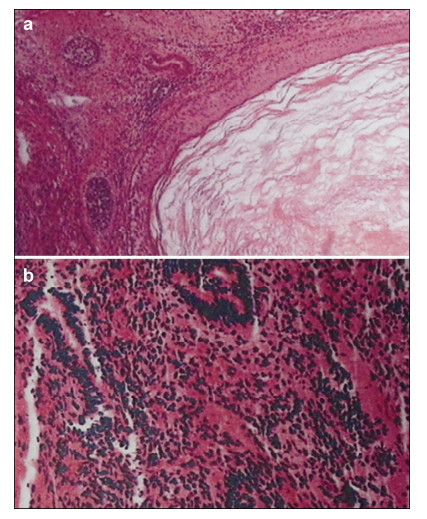
after the operation. Pathological examination revealed
mixed germ cell tumor (
Figures 8a and
8b).
2 Discussion
Intracranial germ cell tumors account for approximately 15% of intracranial primary tumors in children,
and there are obvious regional differences
[1, 2, 3, 4]. Common
sites of intracranial germ cell tumors include the pineal
region and sellar area,basal ganglia area,cavernous
sinus area,posterior fossa,and brainstem
[5, 6, 7, 8]. Different
locations have different symptoms. The tumor may
appear cystic,heterogeneous,and full of solids in
MRI
[4, 5, 6, 7, 8]. Intracranial germ cell tumors can also be
divided into germinomatous and nongerminomatous
germ cell tumors. The latter can be further divided into
teratoma,choriocarcinoma,endodermal sinus tumor,
embryonal carcinoma,and mixed germ cell tumor
[9].
Mixed germ cell tumor is a common classification,in
which the internal components of the tumor are
complex. Germ cell tumors can rapidly increase in
size due to chemotherapy or radiotherapy
[9, 10, 11, 12, 13]. Tumors
that rapidly increase in size without special treatment
are rarely reported.
The pathological findings in this case showed a
mixed germ cell tumor. There was no obvious change
in the imaging features of the tumor since diagnosis 3
years prior. However,after the onset of new symptoms,
MRI showed that the tumor composition and volume
had significantly changed. It has been reported that
benign teratomas can relapse into malignant tumors
after total resection,and some scholars have speculated that the pathology may be incomplete[13, 14].
Combining the characteristics of this case and related
literature,we speculated that benign tumors may
later relapse into malignant ones,and the inconsistent
pathologic results are not due to incomplete specimens[15].
It is necessary to examine the serum tumor markers,
as the abnormal changes in serum tumor markers are
often earlier than the imaging changes[16]. This patient
only previously experienced a ventriculo-peritoneal
shunt,and there was a lack of evidence for serum
tumor markers.
Biopsy surgery should be avoided as far as possible
with this type of tumor[17]. First,there is a high risk
of tumor hemorrhage after surgery. Second,the
pathological findings of a biopsy are limited due
to the diversity of the intracranial germ cell tumors’
internal components[9]. In our cases,we have concluded that intracranial germ cell tumors are likely to
have a malignant transformation at any time,and
this may significantly increase the risk of treatment.
Therefore,palliative treatment is not indicated with
this kind of tumor; instead,the tumor should be
aggressively resected as early as possible. The different
subtypes of germ cell tumors can be classified according to the results of preoperative tumor marker tests,
which can guide treatment,especially the choice of
treatment programs.
Tumors located in the posterior part of the third
ventricle are more anatomically complex,and operation
risk is very high. The most variable factor affecting
prognosis of the disease is surgical skill—if the operator
is skilled,neurological function will be well protected
and good therapeutic effects will be achieved[18, 19].
Preoperative MRI examination and some special MRI
sequences are helpful to understand the characteristics
of the tumor,the relationship between the tumor and
the nerves and blood around it,and the internal blood
supply of the tumor. More complete understanding
can greatly reduce the risk of surgery.
The most commonly used surgical approach for
third ventricle tumors is the corpus callosum dome,
which cuts part of the corpus callosum and separates
the dome. Zhang et al. believes that cognitive function
will be less affected in patients experiencing a corpus
callosotomy within 2.5 cm in length[20]. However,
our patients have short-term memory disorder after
surgery; we speculated that this was related to fornix
injury. Diffused tension image (MRI-DTI) sequence
examinations can be performed before and after surgery to examine the nerve fibers of the corpus callosum
and fornix. This may be helpful for evaluating the
patient’s postoperative cognitive function.
In patients with mixed germ cell tumor,the tumor
should be resected as much as possible. Our patient’s
tumor was totally removed,with an intact capsule.
This indicated a good prognosis. Although the tumor
was completely removed,tumor marker values were
still higher than normal,indicating the existence of
malignant tumor cells; therefore,chemotherapy treatment was necessary after surgery. After chemotherapy,
there may be necrosis of the residual tumor in MRI
scans,and serum tumor markers may return to normal.
However,there is much controversy about when to
choose chemotherapy for germ cell tumors,since
chemotherapy can cause tumor constituent changes[21].
This will then affect the choice of treatment programs.
Based on experience,we recommend that only diagnosed patients or tumors with rich blood supply be
chosen for chemotherapy treatment,and only as an
auxiliary postoperative treatment.
Mixed germ cell tumors are not sensitive to
radiotherapy[22],which may cause a tumor’s malignant transformation and abrupt enlargement[9]. This
may cause the patient to lose the treatment opportunity
and is not recommended as the routine treatment.
In short,for mixed germ cell tumors,combined with
Doctor Zhang Yuqi’s long clinical experience[23, 24, 25, 26, 27],
we make the following recommendations. First,a
complete pre-operative examination must be done,
especially for serum tumor markers that will aid in
correct diagnosis and treatment. Additionally,good
surgical technique is key to the treatment of mixed
germ cell tumor. The fundamental treatment for nongerminomatous germ cell tumors is surgical removal.
Total tumor resection is an important variable affecting
prognosis. Chemotherapy is also an important treatment for mixed germ cell tumor; early postoperative
chemotherapy is very important. Because of its serious
side effects,including bone marrow suppression,
low immunity,and changes in the nature of tumor
pathology,chemotherapy is not recommended as the
first choice,and instead is mainly used as an adjunctive postoperative treatment for tumors with definite
pathological results. For mixed germ cell tumor,
radiotherapy is not chosen as a common treatment.
We also recommend serum tumor marker examination
during follow up.
Conflict of interests
The authors have no financial interest to disclose
regarding the article.