2. Department of Neural Reconstruction, Beijing Neurosurgery Institute, Capital Medical University, Beijing 100050, China
The distribution of cavernous malformations (CMs) within the central nervous system is proportional to the volume of different compartments[1]. Regarding CMs in the suprasellar region, a hypothalamic CM is extremely rare, even when compared with the infrequent CM in the optic pathway[2-6]. Further, the anatomical location and eloquence of critical neural structures make this deeply located CM difficult to access surgically and remove[7-11]. Here, we present a very rare case of CM in the hypothalamus, which was totally excised using a right pterional approach, with a satisfactory outcome; no regrowth has been seen on follow-up Magnetic resonance imaging (MRI) over the course of 2 years.
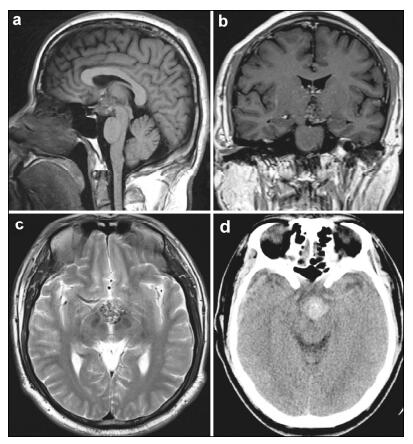
2 Case presentationA 40-year-old male, who complained of impaired vision in the left eye for a year and a half, was hospitalized for further examination of a suprasellar region mass detected at his local hospital. He was otherwise healthy and had no significant past medical history or history of trauma or surgery. Eye examination showed his best-corrected visual acuity was 0.8 in the left eye and no obvious abnormality in the right eye. He demonstrated no visual field defect or any other symptoms. No other neurological abnormalities were found. The pituitary hormonal examination and physical examination were normal. Computed tomography (CT) demonstrated a mass located in the suprasellar region. MRI on admission demonstrated a 2.2 mm × 2.5 mm × 2.1 mm regular-shaped round lesion located in the suprasellar cistern, to the rear of the optic chiasm. The lesion showed upward extension into the third ventricle. T1-and T2-weighted images showed mixed signal intensity with no edema around the lesion. A contrast-enhanced scan showed a hetero geneous mild enhancement (Figure 1).
|
| Figure 1 Magnetic resonance imaging (MRI) and computed tomo graphy (CT) of the presurgical hypothalamic cavernous malformation. (a) Sagittal section of T1-weighted MRI shows mixed-signal, round lesions located in the suprasellar cistern. (b) Coronal section of gadolinium-enhanced T1 images show a heterogeneous mild enhancement of the lesion located in hypothalamus. (c) Axial section of T2-weighted MRI shows the lesion’s upward extension into the third ventricle. There was no typical hypointense signal rim around the lesion. (d) Unenhanced computed tomographic imaging reveals a hyperdense lesion in the suprasellar region. |
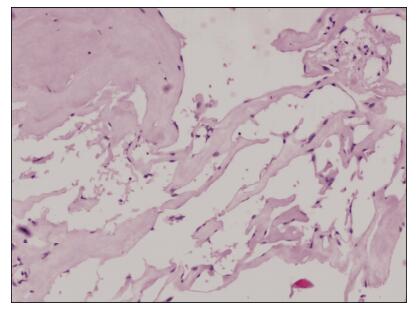
Consequently, the patient was treated with micro surgical dissection via right pterional craniotomy. During the surgery, we confirmed that the lesion was located in the suprasellar region, broke upward into the third ventricle and downward into the inter peduncular cistern. The lesion was gray-red in color, soft but solid, covered by a membrane, and with a rich blood supply from the right posterior cerebral artery. The upper part of the lesion was embedded in the hypothalamus and caused slight compression of the optic chiasm and optic tract. We completely removed the lesion between the optic nerves and internal carotid artery. The pituitary stalk could not be protected completely because of the close adhesion and massive invasion of the lesion. All other peripheral tissues remained intact, including the brain paren chyma, anterior cerebral artery, basilar artery, posterior cerebral artery, optic nerve, optic chiasm, and oculo motor nerve. Pathological examination confirmed that the surgical specimen was CM (Figure 2).
|
| Figure 2 Photomicrograph shows thin-walled cavernous vascular spaces with little intervening brain tissue (Hematoxylin-eosin stain, ×100). |
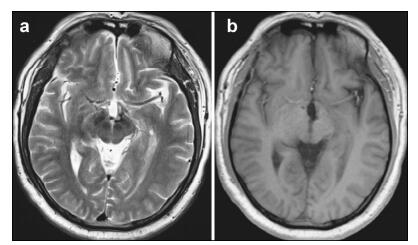
Postoperatively, the patient reported no further visual acuity or field deficits. However, he presented with a temporary electrolyte disorder characterized by fluctuation in the concentration of serum sodium. After fluid replacement therapy and oral hormone supplementation, he recovered well, without any neurological deficits. Postoperative MRI revealed com plete excision of the CM without destruction of the surrounding structures. The two years of follow-up found change in visual acuity or CM recurrence on MRI (Figure 3).
|
| Figure 3 Magnetic resonance imaging (MRI) of the postsurgical hypothalamic cavernous malformation at two-year follow-up. Axial section of T2-weighted (a) and gadolinium-enhanced T1-weighted (b) MRI reveals the complete removal of the hypothalamic cavernous malformation and no evidence of recurrence or rebleeding. |
Intracranial CMs represent 10%-20% of all vascular malformations[1, 12]. Only five cases of CM in the hy pothalamus have been reported among all infrequent CM types[4], and all these cases were in Asian populations[10, 13-15]. Here, we report a hypothalamic CM in a male patient presenting with visual disturbance. Notably, the CM occupied the whole suprasellar region and involved critical and vulnerable structures, including the pituitary stalk, as well as optic chiasm and optic tract, which presents a challenge for neurosurgeons and makes this case special. We are interested in reporting this case to enrich the understanding of the surgical management of hypothalamic CM.
The center of a CM usually contains methemoglobin surrounded by a hemosiderin ring. On MRI images, a CM generally appears with mixed signal intensity and a hypointense rim, called the “iron ring sign”, which shows mild or no enhancement on contrast-enhanced MRI scanning. In this case, the CM presented as a focal round mass. No obvious optic nerve thickening indicated that the mass did not originate from optic nerve or tract, and we speculated that the absence of the typical hypointense rim of the CM may have been due to blood washout by cerebrospinal fluid. To date, hypothalamic CM had been reported to present no clinical features related to hypothalamic dysfunction. Because of the optic involvement, the most common presenting symptom was visual disturbance. Visual acuity loss may occur separately, as shown in this case, or be accompanied by a visual field defect. Bitemporal hemianopia indicates chiasmal involvement, while homonymous hemianopia mostly results from optic tract involvement. Importantly, the protection against and improvement of visual deficits is one of the most critical considerations in therapeutic outcomes[3, 4, 7, 16]. Other symptoms include non-characteristic headache, retroorbital pain, and weakness, and the onset of symptoms can occur in both acute and progressive manners. In most instances, the com bination of the typical symptoms and MRI results can clarify the characterization of CM[1]. However, a confirmed diagnosis of hypothalamic CM is still hard to reach due to its extremely low incidence. It is important to emphasize the differential diagnosis including other tumors in the suprasellar region, such as glioma, germ cell, craniopharyngioma, pituitary adenoma, and metastatic tumors.
The natural history of CM has been reported to vary with the location of the lesion. We have speculated on the clinical characteristics of hypothalamic CMs from other CMs in suprasellar region according to the nearby location. Compared with supratentorial com partment lesions, deep-seated CMs, including CMs in the brain stem, basal ganglia, ventricles, or optic chiasm, are prone to bleeding and stroke[3, 7, 9, 17-19]. Although the hemorrhage and rehemorrhage rates for hypothalamic CM are not known, it is reasonable to consider that hypothalamic CM has higher bleeding and rebleeding rates because of the same eloquent location. Based on the fact that this young patient had a large and symptomatic CM in the hypothalamus, and waiting unnecessarily increases the risk of bleeding, further lesion growth, or hydrocephalus, we suggested that complete surgical excision is the appropriate therapeutic approach, as recommended in previous studies[3, 4, 9, 20]. In some cases, the CM could involve multiple deep brain structures, presenting a hazardous situation[10, 13]. However, consistent with all other surgical approaches to treating CMs, the crucial issue is complete excision of the whole CM with proper protection to the surrounding healthy brain structures. Moreover, any residual malformation often causes further rebleeding and recurrence and can be fatal for CMs located in deep brain structures[14, 19]. Sharp dissection and block resection of the CM often lead to unmanageable bleeding and partial excision. Therefore, during the reported surgery, we gently traced the whole border of CM to confirm the dissection plane, especially during dissection of the upper part embedded in the hypothalamus, and we finally completed the full removal of the CM at the expense of irreparable damage to the pituitary stalk, rather than risking partial excision. With the aim of gross-total resection and minimal manipulation of the surround ing normal tissue, we used pterional craniotomy to provide a wide surgical field to facilitate approaching the lesion.
During the two years of follow-up with no evidence of recurrence or rebleeding, we feel we may make constructive comments on treatment strategies for hypothalamic CM. In summary, accurate preoperative diagnosis with complete surgical removal by an appropriate surgical approach can contribute to satisfactory outcomes.
Conflict of interestsThe authors have no financial interest to disclose regarding the article.
| [1] | Batra S, Lin D, Recinos PF, Zhang J, Rigamonti D. Cavernous malformations:Natural history, diagnosis and treatment. Nat Rev Neurol , 2009, 5 (12) : 659–670. DOI:10.1038/nrneurol.2009.177 |
| [2] | Hassler W, Zentner J, Wilhelm H. Cavernous angiomas of the anterior visual pathways. J Clin Neuroophthalmol , 1989, 9 (3) : 160–164. |
| [3] | Mizutani T, Goldberg HI, Kerson LA, Murtagh F. Cavernous hemangioma in the diencephalon. Arch Neurol , 1981, 38 (6) : 379–382. DOI:10.1001/archneur.1981.00510060081017 |
| [4] | Reyns N, Assaker R, Louis E, Lejeune JP. Intraventricular cavernomas:Three cases and review of the literature. Neurosurgery , 1999, 44 (3) : 648–654. DOI:10.1097/00006123-199903000-00119 |
| [5] | Samii M, Eghbal R, Carvalho GA, Matthies C. Surgical management of brainstem cavernomas. J Neurosurg , 2001, 95 (5) : 825–832. DOI:10.3171/jns.2001.95.5.0825 |
| [6] | Abou-Al-Shaar H, Bahatheq A, Takroni R, Al-Thubaiti I. Optic chiasmal cavernous angioma:A rare suprasellar vascular malformation. Surg Neurol Int , 2016, 7 (Suppl 18) : S523–S526. |
| [7] | Liu JK, Lu Y, Raslan AM, Gultekin SH, Delashaw JB Jr. Cavernous malformations of the optic pathway and hy-pothalamus:Analysis of 65 cases in the literature. Neurosurg Focus , 2010, 29 (3) : E17. DOI:10.3171/2010.5.FOCUS10129 |
| [8] | Mizoi K, Yoshimoto T, Suzuki J. Clinical analysis of ten cases with surgically treated brain stem cavernous angiomas. Tohoku J Exp Med , 1992, 166 (2) : 259–267. DOI:10.1620/tjem.166.259 |
| [9] | Kurokawa Y, Abiko S, Ikeda N, Ideguchi M, Okamura T. Surgical strategy for cavernous angioma in hypothalamus. J Clin Neurosci , 2001, 8 (Suppl1) : 106–108. |
| [10] | Katayama Y, Tsubokawa T, Maeda T, Yamamoto T. Surgical management of cavernous malformations of the third ventricle. J Neurosurg , 1994, 80 (1) : 64–72. DOI:10.3171/jns.1994.80.1.0064 |
| [11] | Rheinboldt M, Blase J. Exophytic hypothalamic cavernous malformation mimicking an extra-axial suprasellar mass. Emerg Radiol , 2011, 18 (4) : 363–367. DOI:10.1007/s10140-011-0940-0 |
| [12] | Gross BA, Du R. Cerebral cavernous malformations:Natural history and clinical management. Expert Rev Neurother , 2015, 15 (7) : 771–777. DOI:10.1586/14737175.2015.1055323 |
| [13] | Simard JM, Garcia-Bengochea F, Ballinger WE Jr, Mickle JP, Quisling RG. Cavernous angioma:A review of 126 collected and 12 new clinical cases. Neurosurgery , 1986, 18 (2) : 162–172. DOI:10.1227/00006123-198602000-00008 |
| [14] | Hempelmann RG, Mater E, Schröder F, Schön R. Complete resection of a cavernous haemangioma of the optic nerve, the chiasm, and the optic tract. Acta Neurochir (Wien) , 2007, 149 (7) : 699–703. DOI:10.1007/s00701-007-1163-8 |
| [15] | Wang CH, Lin SM, Chen Y, Tseng SH. Multiple deep-seated cavernomas in the third ventricle, hypothalamus and thalamus. Acta Neurochir (Wien) , 2003, 145 (6) : 505–508. |
| [16] | Ogawa Y, Tominaga T. Sellar and parasellar tumor removal without discontinuing antithrombotic therapy. J Neurosurg , 2015, 123 (3) : 794–798. DOI:10.3171/2014.9.JNS141088 |
| [17] | Hasegawa H, Bitoh S, Koshino K, Obashi J, Kobayashi Y, Kobayashi M, Wakasugi C. Mixed cavernous angioma and glioma (angioglioma) in the hypothalamus-Case report. Neurol Med Chir (Tokyo) , 1995, 35 (4) : 238–242. DOI:10.2176/nmc.35.238 |
| [18] | Robinson JR, Awad IA, Little JR. Natural history of the cavernous angioma. J Neurosurg , 1991, 75 (5) : 709–714. DOI:10.3171/jns.1991.75.5.0709 |
| [19] | Porter RW, Detwiler PW, Spetzler RF, Lawton MT, Baskin JJ, Derksen PT, Zabramski JM. Cavernous malformations of the brainstem:Experience with 100 patients. J Neurosurg , 1999, 90 (1) : 50–58. DOI:10.3171/jns.1999.90.1.0050 |
| [20] | Lehner M, Fellner FA, Wurm G. Cavernous haemangiomas of the anterior visual pathways. Short review on occasion of an exceptional case. Acta Neurochir (Wien) , 2006, 148 (5) : 571–578. DOI:10.1007/s00701-006-0751-3 |



