Shiting Li achieved the Ph.D. degree in 2001 and has been working in Xinhua Hospital as the chairman of the Neurosurgical Department since 2005. He is the Director of the Cranial Nerve Disease Center of Shanghai Jiaotong University, Leader of Shanghai Functional Neurosurgical Association, Vice-chairman of Chinese Neurological Minimal-Invasive Therapy Association. In 2017, he has established the World Neurosurgeon Federation of Cranial Nerve Disorders and became the first rotating president. With Drs. Zhong and Sekula (from UPMC), he edited a textbook entitled Microvascular Decompression Surgery, in which the most famous experts in this filed around the world contributed chapters.
Although microvascular decompression (MVD) is widely accepted as the most reasonable technique for treating cranial nerve hyperexcitability disorders, such as trigeminal neuralgia, hemifacial spasm, etc., it is still a risky procedure due to the delicate cerebellopontine structures. In some cases, patients are not totally relieved of their symptoms postoperatively[1, 2], and thus, this surgical technique needs to be further refined. In the current paper, we shared our experience with more than 10, 000 MVDs[3, 4].
Most operators are inclined to focus on microscopic dissections, leaving earlier procedures to their residents. However, these procedures, such as positioning, incision, and craniectomy, actually compose a necessary precondition for proper exposure.
The patient should ideally be placed at a 3/4 lateral prone decubitus, since this position is superior to supine or full prone position because it obviates the need to turn the patient's head into an uncomfortable position. This subsequently decreases the risk of postoperative neck pain, especially for obese patients with generous supraclavicular fat pads. It is important to place the contralateral shoulder close to the edge of the bed and to pull the ipsilateral shoulder away from the head by a shoulder belt; this will facilitate the instruments getting in and out of the surgical field for the operator. A fixation frame is suggested to hold the patient's head stable. We preferred to keep the patient's head at an oblique position, i.e., turning it back 15°. With this position, the cerebellum may fall away under its own gravity from the petrosal bone, obviating the need for retractors.
A craniectomy that is lateral enough to expose the sigmoid sinus is necessary to achieve a satisfactory surgical corridor. To avoid dural sinus injury, the bone over the sigmoid sinus should be removed in small pieces. Accordingly, a craniectomy with a pneumatic drill and Kerrison Rongeur is superior to a craniotomy with milling cutters. To obtain a good working angle, the operator should not hesitate to open the mastoid antrum if necessary, but it should be immediately waxed to prevent infection and cerebrospinal fluid (CSF) leak.
Usually, unhurried suction drainage of CSF and an ample adhesiolysis, with thorough arachnoid dura opening, are effective enough to achieve brain relaxation. Mannitol or a lumbar puncture is not required for most cases. We do not use retracting blades because, in comparison to a wider spatula, a narrow suction tube allows more mobility and actually affords more working space at the moment when a specific area is dissected. A good knowledge of the regional anatomy means that one does not have to visualize the whole area of the cerebellopontine angle while operating at a particular site (but one needs to be mindful of the surrounding structures).
A caudorostral approach is suggested.
In hemifacial cases, it is very common that the neurovascular conflict occurs in the caudal root exit zone (REZ) of facial nerve root. Sometimes, the offending artery can even be buried under the caudal cranial nerves. Therefore, the dissection should start from the caudal nerves and move rostromedially to the pontomedullary sulcus.
In trigeminal cases, the protection and management of petrosal veins poses the main challenges and risks during the process. To detour off the petrosal veins, the arachnoid membranes around the petrous and the superior cerebellopontine fissures should be dissected sharply. Generally, the REZ of the Ⅴ nerve will be directly in your sight with the cerebellar fissures opened thoroughly[5].
Generally, skillful driving of a micro dissector to assist with a fine suction tube using the operator's two hands is enough to complete the decompression process, including removal of the offending vessel (s) and placement of Teflon wadding piece by piece. No other instruments controlled by a third hand are needed in such a small room. Moving vessels with forceps is not recommended. The purpose of decompression is to separate the neurovascular confliction, rather than to insert with prosthesis, between the nerve and the vessel. The role of the Teflon is to keep the offending vessel from rebounding. Therefore, it is unnecessary to always put the Teflon at the site of conflict[1]. Furthermore, the offending arteries should be positioned anatomically.
Encountering a tortuous vertebrobasilar artery complex (VBA) during the MVD can be challenging[6, 7]. In these cases, the point of the surgery is to move the proximal VBA before dissection of the facial or trigeminal nerve. It should be mobilized caudolaterally, with gradual placement of small pieces of shredded Teflon between the VBA and the medulla oblongata through the interstices of the caudal cranial nerves. Afterwards, the neurovascular conflict can be distinguished without difficulty in most of cases.
Since MVD is a functional surgery, it should be as safe as possible[8]. Therefore, it is recommended to end the operation if an apparent offending artery is found in the axilla of the Ⅶ nerve, especially if a dent is also visualized in the nerve and the abnormal muscle response vanishes when the artery is removed. If symptoms do not improve at all, postoperatively, an immediate reoperation with exploration of the entire intracranial segment of the facial nerve should not be rejected, as long as the patient does expect immediate relief. For trigeminal cases, the entire intracranial course of the Ⅴ nerve should be exposed as much as possible to clear off all the vessels from the nerve[5, 9].
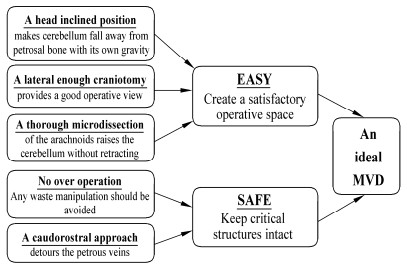
In order to achieve an effective and safe MVD, any waste procedures should be avoided intraoperatively[10]. Basically, a head-inclined position, lateral enough craniotomy, and thorough microdissection may cause the cerebellum fall away from the petrosal bone with its own gravity and create a satisfactory working space for vascular decompression, with no requirement for retractors[3]. Furthermore, a caudorostral approach may not only detour the petrous veins but also reach the neurovascular conflict more directly[5] (Figure 1).
|
| Figure 1 A sketch demonstrating the ideal microvascular decompression surgery (MVD) technique, which should be easy and safe. |
Conflict of interests
All contributing authors have no conflict of interests.
| [1] | Dou NN, Zhong J, Liu MX, Xia L, Sun H, Li B, Li ST. Teflon might be a factor accounting for a failed microvascular decompression in hemifacial spasm: A technical note. Stereotact Funct Neurosurg, 2016, 94(3): 154–158. DOI:10.1159/000446192 |
| [2] | Zhong J, Xia L, Dou NN, Ying TT, Zhu J, Liu MX, Li ST. Delayed relief of hemifacial spasm after microvascular decompression: Can it be avoided?. Acta Neurochir, 2015, 157(1): 93–99. DOI:10.1007/s00701-014-2247-x |
| [3] | Zhong J, Zhu J, Sun H, Dou NN, Wang YN, Ying TT, Xia L, Liu MX, Tao BB, Li ST. Microvascular decompression surgery: Surgical principles and technical nuances based on 4000 cases. Neurol Res, 2014, 36(10): 882–893. DOI:10.1179/1743132814Y.0000000344 |
| [4] | Zhong J, Li ST, Zhu J, Guan HX, Zhou QM, Jiao W, Ying TT, Yang XS, Zhan WC, Hua XM. A clinical analysis on microvascular decompression surgery in a series of 3000 cases. Clin Neurol Neurosur, 2012, 114(7): 846–851. DOI:10.1016/j.clineuro.2012.01.021 |
| [5] | Zhu J, Zhong J, Jiao W, Zhou QM, Guan HX, Dou NN, Wang YN, Xia L, Li ST. Via-cerebellar-fissures approach for microvascular decompression of trigeminal nerve. J Craniofac Surg, 2014, 25(4): 1438–1440. DOI:10.1097/SCS.0000000000000780 |
| [6] | Li ST, Zhong J, Sekula RF Jr. Microvascular Decompression Surgery. Netherlands: Springer, 2016. |
| [7] | Guan HX, Zhu J, Zhong J. Correlation between idiopathic hemifacial spasm and the MRI characteristics of the vertebral artery. J Clin Neurosci, 2011, 18(4): 528–530. DOI:10.1016/j.jocn.2010.08.015 |
| [8] | Zhong J. An ideal microvascular decompression technique should be simple and safe. Neurosurg Rev, 2012, 35(1): 137–140. DOI:10.1007/s10143-011-0366-x |
| [9] | Zhong J, Zhu J, Li ST, Guan HX. Microvascular decompressions in patients with coexistent hemifacial spasm and trigeminal neuralgia. Neurosurgery, 2011, 68(4): 916–920. DOI:10.1227/NEU.0b013e318208f5ac |
| [10] | Dou NN, Hua XM, Zhong J, Li ST. A successful treatment of coexistent hemifacial spasm and trigeminal neuralgia caused by a huge cerebral arteriovenous malformation: A case report. J Craniofac Surg, 2014, 25(3): 907–910. DOI:10.1097/SCS.0000000000000567 |



