2. Department of Nephrology, Beijing Luhe Hospital, Capital Medical University, Beijing 101149, China;
3. Department of Psychiatry, Zaozhuang Mental Health Center, Zaozhuang 277103, China;
4. Department of Neurosurgery, The Fifth People's Hospital of Datong, Regional Medical Center Of Shanxi Province, Datong 037006, China
Since September 2015, he has been working at the Department of Neurosurgery at the Beijing Tsinghua Changgung Hospital, School of Clinical Medicine at Tsinghua University.
He specializes in spine and spinal cord diseases, including Chiari malformation, syringomyelia, spinal cord tumors, lumbar spondylosis, and cervical spondylosis. At present, he has published 5 papers that are available in the Science Citation Index, 15 papers in core Chinese journals, and 3 bibliographic books. He has managed 2 National Natural Science Fund Projects and 1 Project from the Ministry of Health, Health Science, and Technology Development.
James Wang is the deputy president and chief physician at the Department of Neurosurgery, Beijing Tsinghua Changgung Hospital, School of Clinical Medicine, Tsinghua University.
Dr. Wang acquired his USA Educational Commission for Foreign Medical Graduatescertified M.D. in 1993 and became an American Association of Neurological Surgeons-certified clinical neurosurgeon in 2003. Since 2010, Dr. Wang has been working as the chief physician at Seattle Providence Hospital and an associate professor at Washington University.
Dr. Wang has extensive experience in the surgical treatment of intracranial tumors, functional neurological diseases, and spine and spinal cord disorders. To date, Dr. Wang has published more than 30 academic articles in both domestic and foreign academic journals.
The O-arm Surgical Imaging System (Medtronic, Louisville, CO, USA) is a multidimensional surgical imaging platform designed for use in surgeries of the spine and brain, and in cases of trauma. The system provides real-time intraoperative imaging of the patient's anatomy through high-quality images and two-/three-dimensional (2D/3D) fields-of-view. By integrating the O-arm surgical imaging technique and the Stealth Station Surgical Navigation System (Medtronic), a surgeon can improve the visibility of complex procedures and ensure surgical accuracy. Our hospital introduced the O-arm and Stealth Station systems in November 2014 and 60 spinal operations have been performed using these instruments to assess their safety and precision. This report describes our experience.
2 Methods and materials 2.1 General informationThe study enrolled 60 spinal internal fixation patients (36 males, 24 females; age range, 8-76 years) who were treated and followed-up between May 1, 2015 and July 1, 2017. The treated conditions included atlantoaxial subluxation (28 cases), cervical kyphosis (4), thoracic intraspinal meningioma (4), lumbar spinal stenosis (8), lumbar spondylolisthesis (10), lumbar vertebral compression fracture (4), lumbar spinal schwannoma (1), and sacrococcygeal chordoma (1). The patients were classified into two groups, according to their lesion type: the occipitocervical fusion and posterior neck fixation group and the thoracic/lumbar/sacral pedicle internal fixation group.
2.2 Methods 2.2.1 Imaging examinationBefore surgery, all patients underwent plain radiography, computed tomography (CT), and plain and enhanced-scan magnetic resonance imaging (MRI).The lesions were well documented. Intraoperatively, 3D O-arm anteroposterior and lateral views were obtained and recorded. Either radiography or CT was repeated 1 month postoperatively to confirm implant locations.
2.2.2 Navigation methodThe O-arm intraoperative imaging system and Stealth Station® S7 surgical navigation system were used. The former included an imaging workstation and ray transmitter, and the later included a computer workstation, navigation system, and infrared positioning system (including reference rack, navigation tracker, wireless navigation guide bar, and adapter). The working principle involves the reference rack being placed on the spinous process of an upper or lower segment of a fixed vertebral body to ensure relative location fixation of the spinous process and reference rack. This also ensures that the infrared positioning signals and the reference rack's receiving device are optimally aligned. After O-arm scanning, the 3D images are imported into the navigation system. After the wireless navigation guide bar has successfully registered in the reference rack registry, the navigation guide bar accuracy is corrected at each exact spinous process locus. After accuracy is established, intuitive real-time navigation is performed.
2.2.3 Surgical methodThe surgery was performed under general anesthesia.The operating table was a Jackson multi-purpose perspective spine bed. The navigation system was placed at the head of the operating table, and the workstation was placed on the side opposite the surgeon.A technician connected the O-arm and navigation systems and entered the patient's information into the system. Before the operation, the O-arm's 2D perspective mode was used for positioning.
Each patient in the occipitocervical fusion group was placed prone, with the head under fixed traction. The occipital bone and cervical posterior structure were visualized through the conventional posteromedial approach. First, posterior cranial fossa suboccipital decompression was performed microscopically, and the navigation reference rack was fixed to the lower vertebral spinous process root of the plant screw. The occipital bone plate was fixed with occipital screws, C2 was fixed with Pars, and the C3, C4, and/or C5 vertebrae were fixed with lateral blocks.
Each patient in the thoracic/lumbar/sacral pedicle internal fixation group was also placed prone. The thoracic/lumbar/sacral posterior structures were revealed through a conventional posteromedial approach, and the navigation reference rack was fixed to the upper vertebral spinous process root of the plant screw. Bilateral pedicle fixation was selected, according to the disease. O-arm scanning produced 2D and 3D anteroposterior and lateral images, which were transmitted to the navigation system workstation. The accuracy of the navigation was verified on the spinous process after the navigation guide bar was registered on the reference rack. The navigator provided many implantation orbits, and the surgeon selected the best one, according to the navigation guide. Screw diameters, lengths, and paths were selected under navigational guidance, and each screw was implanted using real-time navigation. After screw implantation, O-arm anteroposterior and lateral 2D and 3D images were again obtained to evaluate the positioning, direction, and depth of each implant.
2.2.4 Evaluation methodScrew position accuracy was determined with reference to Richter's four classification criteria. (1) We evaluated the accuracy of the lateral block or pedicle screws according to the patient's intraoperative O-arm 3D images, assigning one of three grades. Grade Ⅰ: the screw position is satisfactory—i.e., the screw did not penetrate the lateral block or pedicle cortex, or it penetrated one or the other only slightly ( < 1 mm).Grade Ⅱ: the screw penetrated the lateral block or pedicle cortex by >1 mm, but did not need to be adjusted. Also, the patient showed no peripheral tissue injury and the screw was stable. Grade Ⅲ: the screw penetrated the lateral block or pedicle cortex by >1 mm, and there was peripheral tissue injury.Alternatively, the screw was unstable and needed to be adjusted. (2) Operation time: the average perscrew implantation time. (3) Frequency, duration, and navigation time of the O-arm scan. (4) The presence of complications, with the reasons for their occurrence.
3 ResultsThere were 32 patients (12 males, 20 females) requiring occipitocervical fusion and posterior neck fixation; a total of 182 cervical screws and 84 occipital screws were implanted. There were 28 patients (15 males, 13 females) requiring thoracic/lumbar/sacral pedicle internal fixation; 148 pedicle screws were implanted.
3.1 Pedicle screw position accuracyIn the occipitocervical fusion group, a total of 182 cervical screws were implanted with navigation assistance, including 64 C2 Pars screws and 118 C3 and/or C4 lateral block screws. Intraoperative O-arm 3D scans revealed 176 Richter grade Ⅰ screws and 6 grade Ⅰ screws penetrating the lateral block cortex near the vertebral artery (Figure 1), yielding an accuracy of 96.7% (176/182). Among the 84 occipital screws, 3 deviated from the occipital posterior midline position, yielding an accuracy of 96.4% (81/84).
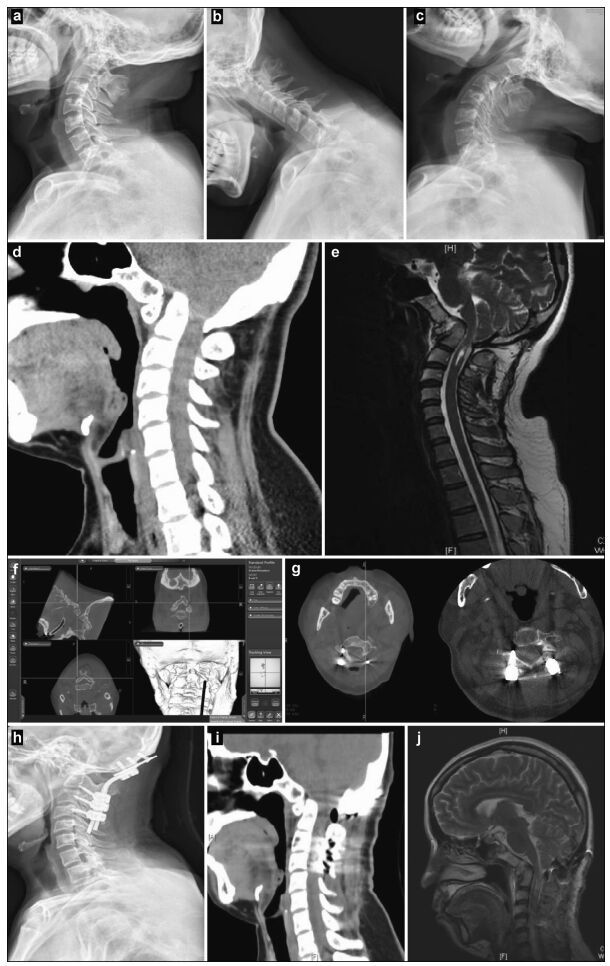
|
| Figure 1 Preoperative, intraoperative, and postoperative images of patients with atlantoaxial dislocation and occipitocervical fusion. Preoperative cervical radiography in the side (a), anteflexion (b), and supine (c) positions reveals odontoid instability and a backward and upward shift. Preoperative computed tomography (CT) (d) and magnetic resonance imaging (MRI) (e) show that the backward and upward dislocation of the C2 odontoid impacts the brain stem. The foramen magnum is narrow, and the cervical cord void is visible. (f) Implantation direction and C2 angle. Pars screws are planed under intraoperative navigation. (g) O-arm three-dimensional scan, after screw implantation, shows that the Pars screw to the right of C2 penetrates the bone cortex and is near the vertebral artery. Lateral radiography (h), sagittal CT (i), and a T2 sagittal scan (j), 1 week after the operation, show firm screw fixation in a good position and inferoanterior displacement of the odontoid to the C1 level, essentially achieving normal anatomical reduction. Brain stem compression is released, and the posterior cranial fossa is fully decompressed. |
For the thoracic/lumbar/sacral pedicle internal fixation group, 148 pedicle screws were implanted under navigational guidance. Intraoperative O-arm 2D lateral scans did not show screw position deviations, but the 3D scans found 148 Richter grade Ⅰ screws (0 screws penetrating the pedicle) and 4 grade Ⅱ screws that had deviated to the lateral pedicle (Figures 2-5).Intraoperative O-arm 3D scans were repeated for confirmation. Secondary correction was performed under navigational assistance, yielding a final accuracy of 97.3% (144/148).
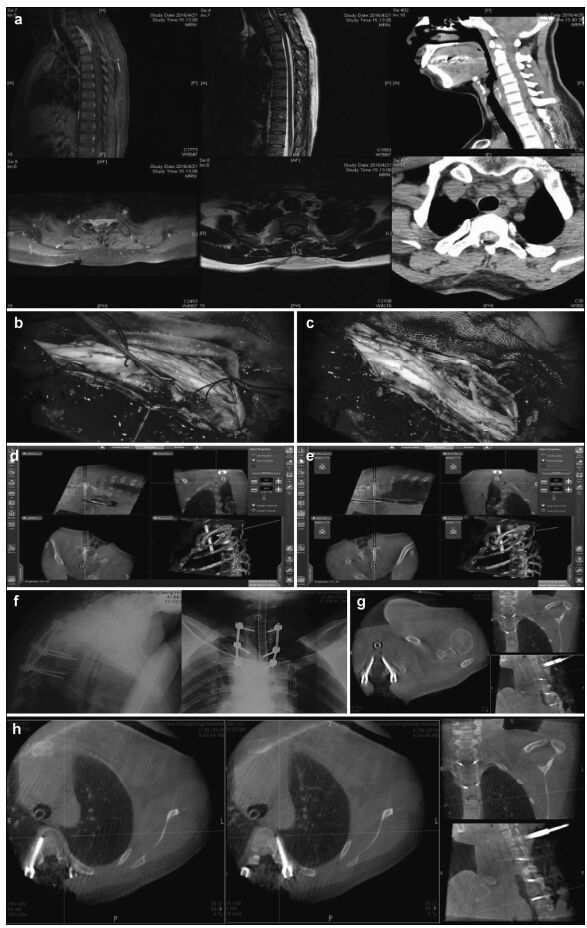
|
| Figure 2 Preoperative, intraoperative, and postoperative images of patients in the thoracic intraspinal meningioma resection and pedicle screw fixation group. (a) Cervical thoracic vertebrae computed tomography shows a high-density tumor shadow in the thoracic spinal canal (T1-T4). Magnetic resonance imaging shows T2 image isointensity in the spinal canal (T1-T4). An enhanced scan shows a significantly enhanced area located in the ventral spinal cord that has invaded the intervertebral foramen. (b) Intraoperative microscopy shows a spinal cord ventral tumor, originating in the dura mater. (c) Intraoperative microscopy shows nearly total resection of the spinal cord ventral tumor, with the spinal cord remaining intact. (d, e) Intraoperative T2 pedicle screw implantation is performed under real-time navigation. The entry direction, angle, and depth of the screw is according to the navigation plan. (f, g, h) After screw implantation, an O-arm two-dimensional lateral scan shows good screw positioning. The O-arm three-dimensional scan found that the T1 bilateral pedicle screws are well positioned and do not penetrate the bone cortex. The T4 left pedicle screw position is also good. The left pedicle screw is in the lateral vertebrae, and no lung injury is seen between the vertebral body and rib. The screw position was not adjusted intraoperatively because it is within the acceptable range. |
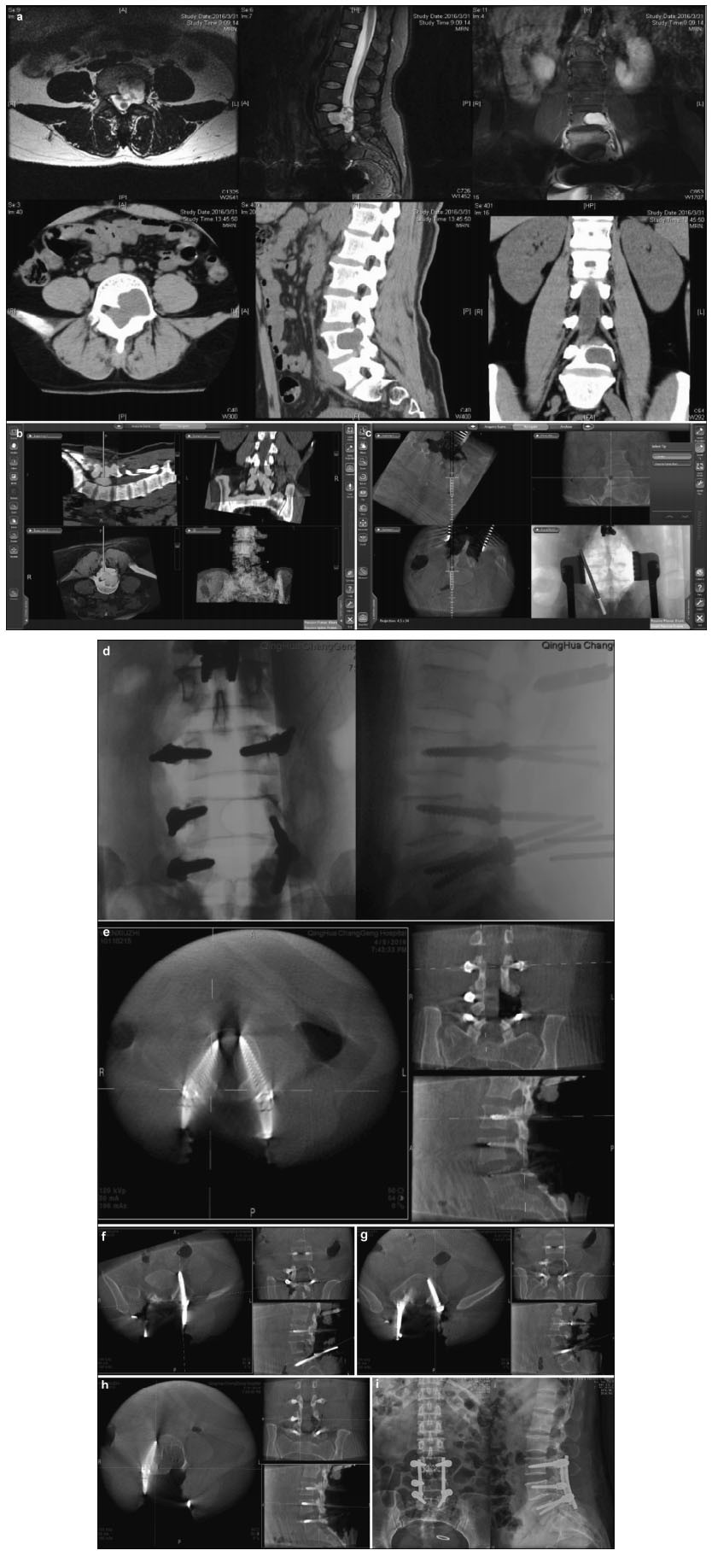
|
| Figure 3 Preoperative, intraoperative, and postoperative images of the lumbar spinal canal of a patient in the internal and external schwannoma resection and pedicle screw fixation group. (a) Lumbar computed tomography (CT) shows an L4-5 intraspinal isodense tumor and a damaged L4 left pedicle and vertebral body. Magnetic resonance imaging (MRI) shows an iso-and hyperintensive signal tumor at L4-5 on the intraspinal T2 image. It is located on the left side of the spinal canal and has invaded a vertebral body and the intervertebral foramen. (b) Fusion of the CT and MRI images, in combination with an intraoperative O-arm and navigation technique, identifies the tumor site and border. (c) Intraoperative L5 pedicle screw implantation is performed under navigation. The screw's direction, angle, and depth can be seen to match the navigation plan. (d) After screw implantation, an intraoperative O-arm two-dimensional lateral scan shows that the screw position is good. (e) An O-arm three-dimensional (3D) scan shows that the L3 pedicle screw position is good, and does not penetrate the bone cortex. (f) An O-arm 3D scan shows that the L5 left pedicle screw position moves away from the vertebral body and penetrates the rough pedicle bone cortex; (g) An O-arm scan was conducted again to introduce the navigation system as part of the correction of the L5 left pedicle screw, getting it to a good position. (h) An O-arm 3D scan shows that the L4 right pedicle screw position is good. It does not penetrate the bone cortex. Screws are difficult to implant in the left pedicle and vertebral body due to tumor invasion. (i) A lateral lumbar radiography scan, 7 days postoperatively, shows firm screw fixation and good positioning. |
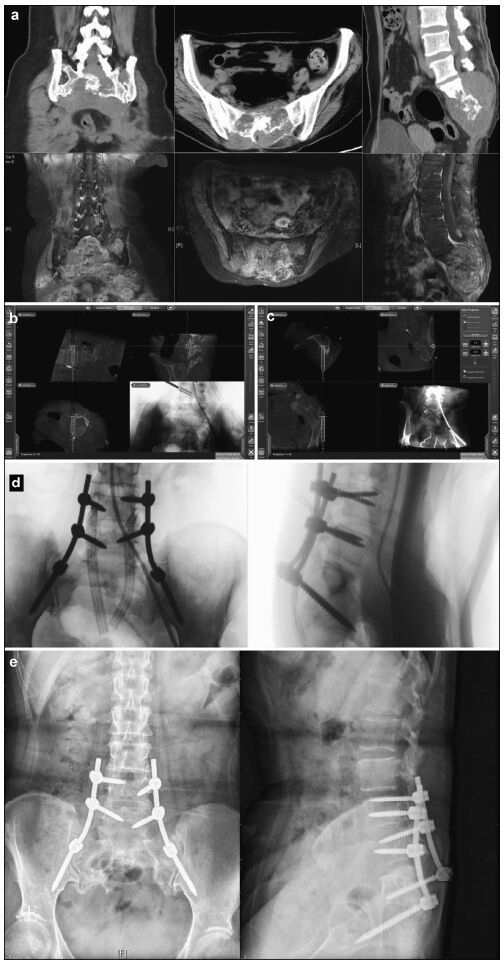
|
| Figure 4 Preoperative, intraoperative, and postoperative images of patients in the nearly total sacrococcygeal chordoma resection and pedicle screw fixation group. (a) Lumbosacral vertebral computed tomography shows an S1-3 intraspinal isodense tumor and a severely damaged vertebral body. An enhanced magnetic resonance imaging scan shows S1-3 intraspinal internal and external tumors and a vertebral body that has been invaded and damaged. (b) Intraoperative L4 left pedicle screw implantation is performed under navigation. The direction, angle, and depth of the screw entery can be seen to match the navigation plan. (c) Intraoperative right iliac screw implantation is conducted under navigation. The direction, angle, and depth of the screw entering can be seen according to the navigation plan. (d) After screw implantation, an O-arm two-dimensional lateral scan shows good screw positioning. (e) A lateral lumbar radiographic scan, 7 days postoperatively, shows firm pedicle and iliac screw fixation and good positioning. |
|
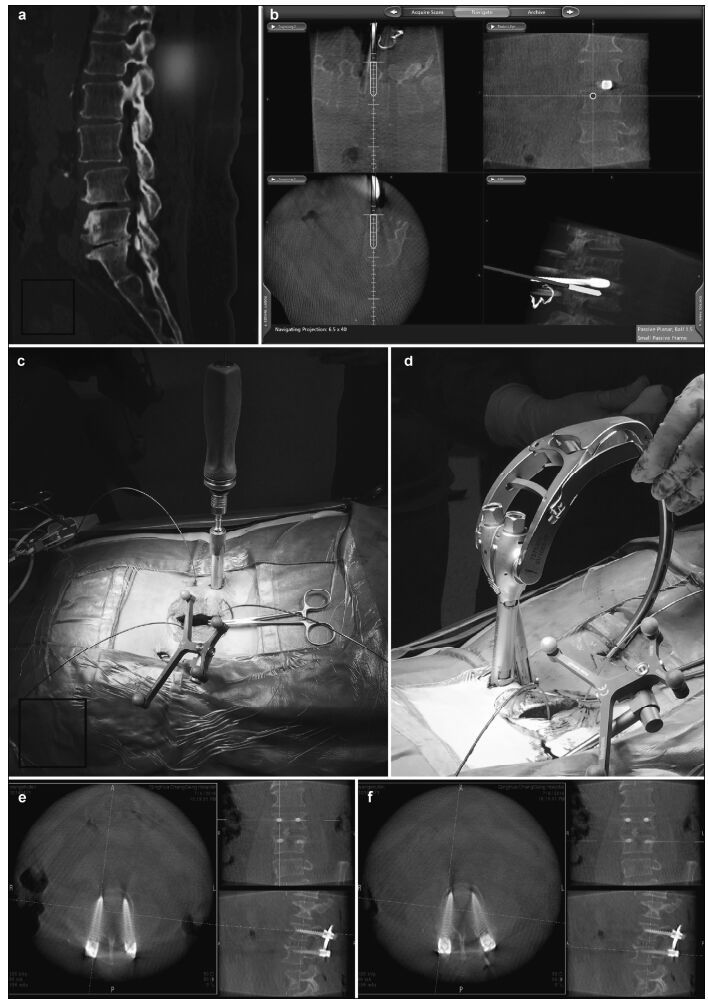
| Figure 5 Preoperative, intraoperative, and postoperative images of patients in the percutaneous minimally invasive pedicle internal fixation group. (a) Lumbosacral vertebral computed tomography shows L3 vertebral spondylolisthesis, L3-4 and L4-5 spinal stenosis, intervertebral disc degeneration, and corresponding intervertebral space narrowing. (b) Intraoperative L4 right pedicle screw implantation is performed under navigation. The direction, angle, and depth of screw entry can be seen in real-time, according to the navigation plan. (c, d) Intraoperative screw implantation and bar threading are performed under navigation. (e, f) After screw implantation, O-arm three-dimensional anteroposterior and lateral scans show that the screw is well positioned. |
In the occipitocervical fusion group, the navigationguided implantation operation time for each cervical spine screw was 5-7 min, with a total implantation time for each occipital screw of 3-5 min. In the thoracic/lumbar/sacral pedicle fixation group, the navigationguided implantation operation time for each thoracic pedicle screw was 8-10 min, with an implantation time for each lumbar pedicle screw of 6-8 min.
3.3 O-arm scan frequency, duration, and navigational timeThe preparation time for starting the O-arm and its navigational equipment, setting parameters, and connecting was 20-30 min/time. The average time for an O-arm anteroposterior and lateral 3D scan and importing these into the navigational system was 3-5 min/time. The average O-arm scan frequency was 3 times/case (including positioning the section, 3D scanning, importing the image into the navigation system, and post-implantation verification). The radiation dose for each 3D scan was approximately 5-7 mSv.
3.4 Immediate complicationsPostoperatively, one occipitocervical fusion patient developed dysphagia and underwent removal of the connecting rod after no improvement was observed within 2 months. The deglutition function gradually recovered over 1 month. This complication is believed to be related to over-flexion of the neck after occipitocervical fusion.
4 DiscussionBoucher et al. first applied the spinal pedicle fusion technique in 1959. Since then, the technique has become prevalent worldwide. However, empirical "blind screwing" positional deviations of approximately 10%-40%[1] result in damage to the nerve/spinal cord/ blood vessels and even to intra-abdominal organs, making the accuracy of pedicle screw implantation a challenge for clinicians. Roberts et al. first applied a neurosurgical navigation technique in 1986[2], which was extended to spinal fixation by Steinmann et al.[3], greatly improving screw implantation accuracy. The current navigation techniques include preoperative CT navigation, isocenter C-arm navigation, and intraoperative O-arm navigation. The latter technique, intraoperative O-arm real-time navigation, is the most advanced of these techniques; however, reaching 100% accuracy is difficult, regardless of the navigation technique employed. We studied the 60 intraoperative O-arm real-time navigation cases performed in our department and analyzed the possible causes of navigation inaccuracy and screw implantation bias.
Much of the literature states that the accuracy of navigation-assisted screw fixation is >90%, which is higher than that of traditional screw implantation, improving safety. Cong et al. examined nine C3-7 pedicle screws implantations involving navigational assistance, and found an accuracy of 90%, compared with an accuracy of 55.6% for non-assisted implantations[4]. Yang et al. reported that the accuracy of C1-2 articular screw fixation was 97.2% in 36 cases involving isocenter C-arm navigation, compared with an accuracy of 91.7% for 48 conventional radiography cases[5]. Tao et al. reported that 99 patients underwent intraoperative three-dimensional fluoroscopic navigation, with an accuracy of 98.5% for 196 C3 screw implantations[6]. In this group of occipitocervical fusion patients, the accuracy of performing cervical lateral blocks and implanting Pars screws was 96.7%. Screws penetrated the bone cortex in six patients, resulting in the screws being near, but not injuring, the vertebral arteries; postoperative neurological dysfunction was not observed. These results are similar to the literature results already discussed.
Screw penetration may be related to excessive screw lengths and to the implantation angle. Although depth measurements may be performed under navigation, "individualizing" the screw model is difficult. Screws that are too short may not achieve biological stability, and those that are too long may result in penetrations. In the future, custom 3D-printed screws may solve this problem. In addition, the deviation between the actual spinal position and the navigational image also leads to decreased accuracy, especially in patients requiring multi-segment screw implantations. Hence, when the intraoperative experience differs from expectations, repeated identification and calibration of the navigation system accuracy is necessary.
Laine et al. reported the accuracy of thoracolumbar and lumbosacral pedicle screws in 100 cases and noted that the ratio between the navigational implantation group and the traditional implantation group was 95.4%:86.6%[7]. Amiot et al. reported a total of 294 thoracic/lumbar/sacral screws in 50 patients in a navigation implantation group and 544 thoracic/ lumbar/sacral screws in 100 patients in a conventional implantation group. Their accuracy rates were 95% and 84%, respectively[8]. Bledsoe et al. reported 150 thoracic pedicle screw implantations in 34 patients, using isocenter C-arm navigation, with an accuracy of 93.3%[9]. The implantation of 278 thoracic/lumbar/ sacral pedicle screws, under intraoperative O-arm navigation, was previously reported to have an accuracy of 96.8%[10]. Further, the accuracy of implanting 68 lumbar pedicle screws, under intraoperative O-arm navigation, was previously reported to be 91.2%[11].
Kosmopoulos et al. retrieved 130 articles and performed a meta-analysis of the accuracy of implanting 37, 337 pedicle screws. Their results showed that the accuracy of screw implantations in the navigation group was 95.2%, and that in the non-navigation group was 90.3%[12]. For the thoracic/lumbar/sacral vertebrae fusion patients in our group, the accuracy of pedicle screw implantation was 97.3%; four screws moved out of the pedicle but did not cause neurological dysfunction. Our results are very similar to those reported in the discussed articles. Therefore, based on the results of this group and previous literature reports, intraoperative screw implantation, under O-arm real-time navigation, is highly accurate and has correspondingly good safety.
The accuracy of screw implantations involving O-arm navigation did not reach 100%, and the screw skewing may be related to several factors, including (1) the difficulty of positioning screws in the vertebral body so that they are completely consistent with the position scanned by the O-arm, considering the impacts of breathing and implantation force; (2) developmental deformities and variations in the lateral blocks or pedicles, vertebral instability, screw slippage; and (3) surgical equipment operation, screw implantation, and navigation system errors.
From the perspective of screw implementation and equipment operation times for the two groups, the average O-arm scan frequency was 3 times/case, with a total duration of equipment use of approximately 25-35 min and an average screw implantation time of 3-10 min. Despite the absence of a traditional screw implementation control group, the frequency of and time required for screw position verification using traditional repeated fluoroscopic guidance would normally be longer. In addition, radiation exposure during screw implantation is an unavoidable clinical problem for both patients and medical staff. Although experienced surgeons can significantly reduce the frequency and duration of fluoroscopic examinations, the frequency and total radiation dose are significantly greater for new doctors or patients suffering from spinal deformities. Lange et al. reported that the radiation dose delivered during an O-arm 3D scan of the thoracic and lumbar spine is about 3-8 mSv. In contrast, the radiation dose associated with a spiral CT scan of the thoracic and lumbar spine is about 18-19 mSv[13]. Zhang et al. reported that the radiation dose of the O-arm in 3D mode is only half that associated with 64-row CT[14]. In this study, the average radiation dose associated with an O-arm 3D scan was approximately 5-7 mSv. Thus, the reduced dose and frequency of imaging greatly reduced the radiation exposure for both patients and medical staff. For long-segment screw implantation surgeries, however, the radiation exposure increases by two or more times that typically associated with 3D scanning and the transmission of data into the navigation system also increases due to O-arm scanning range restrictions. Together, these factors increase operation duration and radiation exposure, indicating the need for further technical refinements.
In short, screw implantation involving O-arm realtime navigation allows observation of the screw angle and depth in real-time, greatly improving implantation accuracy and safety, reducing surgeon and patient exposure to radiation, and shortening the time required for new doctors to learn screw implantation techniques. Finally, these types of navigation techniques will be useful for percutaneous, minimally invasive screw implantations and for endoscopic techniques, which are gradually increasing in frequency. This technique further improves the accuracy of a minimally invasive technology.
AcknowledgementsThis project was supported by the Beijing Tsinghua Changgung Hospital Fund (No. 12015C1045). The authors thank Peihai Zhang and Linkai Jing for collecting the archived data and Guihuai Wang and Jin Wang for technical help.
Conflict of interestsNone of the contributing authors have conflicts of interest.
| [1] | Odgers IV CJ, Vaccaro AR, Pollack ME, Cotler JM. Accuracy of pedicle screw placement with the assistance of lateral plain radiography. J Spinal Disord, 1996, 9(4): 334–338. |
| [2] | Roberts DW, Strohbehn JW, Hatch JF, Murray W, Kettenberger H. A frameless stereotaxic integration of computerized tomographic imaging and the operating microscope. J Neurosurg, 1986, 65(4): 545–549. DOI:10.3171/jns.1986.65.4.0545 |
| [3] | Steinmann JC, Herkowitz HN, El-Kommos H, Wesolowski DP. Spinal pedicle fixation. Confirmation of an image-based technique for screw placement. Spine, 1993, 18(13): 1856–1861. DOI:10.1097/00007632-199310000-00022 |
| [4] | Cong Y, Bao NR, Zhao JN, Mao GP. Comparing accuracy of cervical pedicle screw placement between a guidance system and manual manipulation:a cadaver study. Med Sci Monit, 2015, 21: 2672–2677. DOI:10.12659/MSM.894074 |
| [5] | Yang YL, Wang F, Han SM, Wang YH, Dong JL, Li LX, Zhou DS. Isocentric C-arm three-dimensional navigation versus conventional C-arm assisted C1-C2 transarticular screw fixation for atlantoaxial instability. Arch Orthop Trauma Surg, 2015, 135(8): 1083–1092. DOI:10.1007/s00402-015-2249-z |
| [6] | Tao X, Tian W, Liu B, Li Q, Zhang G. Accuracy and complications of posterior C2 screw fixation using intraoperative three-dimensional fluoroscopy-based navigation. Chin Med J, 2014, 127(14): 2654–2658. |
| [7] | Laine T, Lund T, Ylikoski M, Lohikoski J, Schlenzka D. Accuracy of pedicle screw insertion with and without computer assistance:a randomized controlled clinical study in 100 consecutive patients. Eur Spine J, 2000, 9(3): 235–240. DOI:10.1007/s005860000146 |
| [8] | Amiot LP, Lang K, Putzier M, Zippel H, Labelle H. Comparative results between conventional and computerassisted pedicle screw insertion in the thoracic, lumbar, and sacral spine. Spine (Phila Pa 1976), 2000, 25(5): 606–614. DOI:10.1097/00007632-200003010-00012 |
| [9] | Bledsoe JM, Fenton D, Fogelson JL, Nottmeier EW. Accuracy of upper thoracic pedicle screw placement using threedimensional image guidance. Spine J, 2009, 9(10): 817–821. DOI:10.1016/j.spinee.2009.06.014 |
| [10] | Oertel MF, Hobart J, Stein M, Schreiber V, Scharbrodt W. Clinical and methodological precision of spinal navigation assisted by 3D intraoperative O-arm radiographic imaging. J Neurosurg Spine, 2011, 14(4): 532–536. DOI:10.3171/2010.10.SPINE091032 |
| [11] | Baaj AA, Beckman J, Smith DA. O-arm-based image guidance in minimally invasive spine surgery:technical note. Clin Neurol Neurosurg, 2013, 115(3): 342–345. DOI:10.1016/j.clineuro.2012.05.007 |
| [12] | Kosmopoulos V, Schizas C. Pedicle screw placement accuracy:a meta-analysis. Spine, 2007, 32(3): E111–E120. DOI:10.1097/01.brs.0000254048.79024.8b |
| [13] | Lange J, Karellas A, Street J, Eck JC, Lapinsky A, Connolly PJ, Dipaola CP. Estimating the effective radiation dose imparted to patients by intraoperative cone-beam computed tomography in thoracolumbar spinal surgery. Spine, 2013, 38(5): E306–E312. DOI:10.1097/BRS.0b013e318281d70b |
| [14] | Zhang J, Weir V, Fajardo L, Lin J, Hsiung H, Ritenour ER. Dosimetric characterization of a cone-beam O-arm Imaging system. J Xray Sci Technol, 2009, 17(4): 305–317. |



