2. Department of Neurosurgery, Beijing Tsinghua Changgung Hospital, School of Clinical Medicine, Tsinghua University, Beijing 102218, China
Since September 2016, he has been a Ph.D. candidate in the Neurosurgery Department of the Beijing Tsinghua Changgung Hospital. His publications include 14 core Chinese journal articles and 5 Science Citation Index articles.
His current main area of research is the clinical diagnosis and treatment of spinal cord diseases.
Guaihuai Wang is the director and chief physician at the Department of Neurosurgery at the Beijing Tsinghua Changgung Hospital, School of Clinical Medicine at Tsinghua University.
Dr. Wang has previously mentored by renown neurosurgeon and academician Zhongcheng Wang and has more than 25 years of experience in the surgical treatment of brain stem and spinal cord tumors, spinal congenital dysplasia, and spinal degeneration diseases.
To date, Dr. Wang has performed approximately 10, 000 operations for spinal cord diseases, including a successful resection of the intramedullary tumor from the medulla oblongata to level T6, which is one of the longest reported tumors in medical history.
Thus far, he has managed 10 funded research projects and published more than 80 articles in both domestic and foreign academic journals.
Ganglioneuroma is a rare (one per million population), differentiated, benign neurogenic tumor which originates from the neuroepithelium along the sympathetic ganglia[1-7]. The tumor is commonly located in the posterior mediastinum and retroperitoneum. The tumor is usually asymptomatic and detected incidentally, therefore it is referred to as an incidentaloma. With the improvements in radiological imaging in the form of computed tomography (CT) and magnetic resonance imaging (MRI), the number of incidentalomas found has increased. Ganglioneuroma is treated and cured by complete tumor resection, although this can occasionally be risky and challenging. Reports in vestigating the imaging features, diagnosis, treatment and prognosis of ganglioneuromasare scarce. In this study, we review the diagnosis and treatment of a patient with a ganglioneuroma.
2 Case presentationA 29-year-old male patient presented with transient pain in the right chest lasting for three days. The patient had no comorbidities and no significant medical or surgical history. A physical examination revealed no abnormalities. The results of routine laboratory tests were within the normal ranges.
The patient underwent a thoracic spinal MRI, which showed a solid, well-defined mass measuring 7.5 cm × 4.2 cm × 1.5 cm, in the right paravertebral region at the T5-T8 level (Figures 1a, 1b, and 1c). The lesion was slightly hypointense on a T1-weighted MRI and slightly hyperintense on a T2-weighted MRI. Following administration of the contrast agent, intravenous gadolinium, the T1-weighted MRI showed that the tumor had heterogenous enhancement and regular borders extended to the T6-T7 neuro foramen on the right.
|
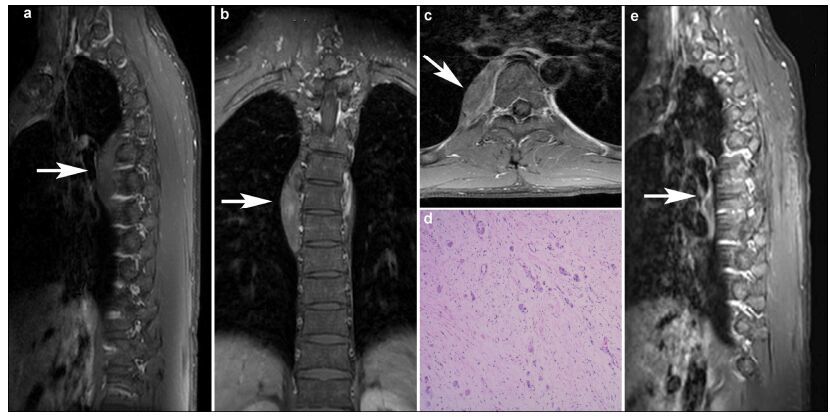
| Figure 1 A 29-year-old male presented with transient chest pain lasting for three days. Magnetic resonance images before surgery (a, b, c) showed a solid, well-defined mass measuring 7.5 cm × 4.2 cm × 1.5 cm, in the right paravertebral region at the T5-T8 level. Histopathological examination (d) confirmed the final diagnosis of ganglioneuroma. No radiological signs of recurrence were observed seventeen months after the surgery (e). |
The preliminary diagnosis was a neurogenic tumor, therefore a surgical resection was performed using a dorsal paramedian approach in the prone position. O-arm (Medtronic, Inc.) intraoperative imaging was used in conjunction with the Stealth Station navigation system (Medtronic Navigation) in order to accurately determine the location of the lesion using real-time intraoperative monitoring. The right transverse processes and costal heads of T6-T7 were removed using an ultrasonic bone curette (MISONIX, Inc.). The tumor was observed at the right side of the T6-T7 vertebrae and was covered with mediastinal pleura. The tumor had a rich blood supply from the mediastinum. In order to prevent neurological complications, we dissected all the adhesions with care and stretched the tumor slightly. A complete en bloc resection was achieved. No related complications occurred.
The tumor was observed to be an encapsulated mass with a solid, homogenous, grayish-tan cut surface. Histopathological examinations led to the final diagnosis of ganglioneuroma (Figure 1d).
The postoperative recovery was uneventful and the patient was discharged on postoperative day seven. On follow-up at seventeen months after surgery, the patient was observed to have no radiological signs of recurrence (Figure 1e).
3 DiscussionNeurogenic tumors of the mediastinum can arise from any tissue of neural crest origin. They are most often located in the posterior mediastinum, and include nerve sheath tumors and nerve cell tumors[3, 8]. Compared with nerve sheath tumors, which account for 40%-65% of neurogenic mediastinal masses, nerve cell tumors are more commonly found in young patients and the majority are malignant[3]. Nerve cell tumors include a spectrum of diseases ranging from purely benign ganglioneuromas to aggressively malignant neuroblastomas. The natural history of suchtumors is unpredictable.
Ganglioneuroma is a benign tumor that is generally develops during childhood, as it originates from the primordial neural crest cells that form the sympathetic nervous system. It is commonly located in the posterior mediastinum and retroperitoneum, as well as the adrenal gland and cervical region[1]. As it is slowly growing and is surrounded by a largecavity, ganglioneuromas are usually asymptomatic in childhood and are usually detected in adulthood. As seen in our case the tumor can cause nonspecific chest pain, or symptoms due to compression of the tracheobronchial tree. Additionally, it may extend to the adjacent intervertebral foramen and invade the spinal canal, leading to cord compression and neurological symptoms.
Ganglioneuroma is usually asymptomatic and detected incidentally. With the recent improvements in radiological imaging, the number of incidentalomas found has increased[2, 5, 8]. On CT, ganglioneuromas predominantly exhibit low to intermediate signal intensity. On T1-weighted MRI images, ganglioneuromasdis play a homogenously low or intermediate signal intensity. On T2-weighted MRI images, they display a heterogeneous, slightly high signal intensity. Although the imaging characteristics of ganglioneuroma have been well described for MRI, it is difficult to precisely diagnose ganglioneuroma using radiological evaluation, prior to surgery.
A posterior mediastinal masspresents with many differential diagnoses. These include a nerve sheath tumor, neuroblastoma, ganglioneuroblastoma, etc.[3-5, 8, 9]. Neurogenic tumors have a wide array of pathologic and clinical features that are classified by the cell type of origin. Nerve sheath tumors are the most common neurogenic tumors in the posterior mediastinum and are often benign, slowly growing, and asymptomatic. Those tumors are usually found in adulthood and most are present for a long period of time prior to diagnosis. Ganglioneuroma, neuroblastoma, and ganglioneuroblastoma are neurogenic tumors with different biological behaviors. Ganglioneuromas arise from the sympathetic ganglia. They display different histological features to other neurogenic tumors, especially to neuroblastomas[4]. The secretion of catecholamines is an uncommon clinical presentation of ganglioneuromas, whereas the majority of the neuroblastomas produce elevated levels of vanillylmandelic acid and homovanillic acid. Thus, urine tests can be used for screening.
There is no gold standard for the treatment of neurogenic tumors. A multidisciplinary, multidepartmental approach is important in order to conduct a thorough preoperative assessment and develop the best treatment strategy. In contrast to neuroblastoma, the treatment of ganglioneuroma is independent of the disease stage. Complete surgical resection (through posterolateral thoracotomy or a dorsal paramedian approach), is the best choice for a curative treatment for mediastinal ganglioneuroma, due to the excellent prognosis[2, 5]. However, surgical morbidity must be considered[7, 10, 11]. To completely remove a ganglioneuroma, which arises from nerve ganglion cells, the involved nerves must also be resected. Due to this, surgery-related complication rate reached 30%[11]. Therefore, watchful waiting or a less radical surgical approach are substitutable options for selected cases. In our case, a complete surgical resection was performed, with a less radical approach in order to protect the adjacent structures and organs.
4 ConclusionGanglioneuroma is a rare benign tumor. Prior to treatment, a careful evaluation using imaging procedures is necessary for an accurate diagnosis. A definitive diagnosis can be made by histological examination. En bloc resection is the preferred treatment for ganglioneuroma, as it has an excellent prognosis.
Conflict of interestsAll contributing authors have no conflict of interests.
| [1] | Kumar S, Singh S, Chandna A. Organ preservation in a case of retroperitoneal ganglioneuroma:A case report and review of literature. Case Rep Surg, 2016: 6597374. |
| [2] | Hayat J, Ahmed R, Alizai S, Awan MU. Giant ganglioneuroma of the posterior mediastinum. Interact Cardiovasc Thorac Surg, 2011, 13: 344–345. DOI:10.1510/icvts.2011.267393 |
| [3] | Reeder LB. Neurogenic tumors of the mediastinum. Seminars in Thoracic and Cardiovascular Surgery, 2000, 12: 261–267. DOI:10.1053/stcs.2000.16738 |
| [4] | Przkora R, Perez-Canto A, Ertel W, Heyde CE. Ganglioneuroma:Primary tumor or maturation of a suspected neuroblastoma?. Eur Spine J, 2006, 15: 363–365. DOI:10.1007/s00586-005-0964-9 |
| [5] | Kizildag B, Alar T, Karatag O, Kosar S, Akman T, Cosar M. A case of posterior mediastinal ganglioneuroma:The importance of preoperative multiplanar radiological imaging. Balkan Med J, 2013, 30: 126–128. DOI:10.5152/balkanmedj. |
| [6] | Yorita K, Yonei A, Ayabe T, Nakada H, Nakashima K, Fukushima T, Kataoka H. Posterior mediastinal ganglioneuroma with peripheral replacement by white and brown adipocytes resulting in diagnostic fallacy from a false-positive 18f-2-fluoro-2-deoxyglucose-positron emission tomography finding:A case report. J Med Case Rep, 2014, 8: 345. DOI:10.1186/1752-1947-8-345 |
| [7] | De Bernardi B, Gambini C, Haupt R, Granata C, Rizzo A, Conte M, Tonini GP, Bianchi M, Giuliano M, Luksch R, Prete A, Viscardi E, Garaventa A, Sementa AR, Bruzzi P, Angelini P. Retrospective study of childhood ganglioneuroma. J Clin Oncol, 2008, 26: 1710–1716. DOI:10.1200/JCO.2006.08.8799 |
| [8] | Ozawa Y, Kobayashi S, Hara M, Shibamoto Y. Morphological differences between schwannomas and ganglioneuromas in the mediastinum:Utility of the craniocaudal length to major axis ratio. Br J Radiol, 2014, 87: 20130777. DOI:10.1259/bjr.20130777 |
| [9] | Meyer S, Reinhard H, Ziegler K, Gottschling S, Aliani S, Krenn T, Graf N. Ganglianeuroma:Radiological and metabolic features in 4 children. Pediatr Hematol Oncol, 2002, 19: 501–508. DOI:10.1080/08880010290097323 |
| [10] | Paasch C, Harder A, Gatzky EJ, Ghadamgahi E, Spuler A, Siegel R. Retroperitoneal paravertebral ganglioneuroma:A multidisciplinary approach facilitates less radical surgery. World J Surg Oncol, 2016, 14: 194. DOI:10.1186/s12957-016-0953-y |
| [11] | Retrosi G, Bishay M, Kiely EM, Sebire NJ, Anderson J, Elliott M, Drake DP, Coppi P, Eaton S, Pierro A. Morbidity after ganglioneuroma excision:Is surgery necessary. Eur J Pediatr Surg, 2011, 21: 33–37. DOI:10.1055/s-0030-1263195 |



