2. Department of Nephrology, Beijing Luhe Hospital, Capital Medical University, Beijing 101149, China;
3. Department of Psychiatry, Zaozhuang Mental Health Center, Zaozhuang 277103, China;
4. Department of Neurosurgery, The Fifth People's Hospital of Datong, Regional Medical Center of Shanxi Province, Datong 037006, China
Since August 2014, he has been a resident at the Neurosurgery Department of the Beijing Tsinghua Changgung Hospital. As a 4th-year resident, he has published 5 core Chinese journal articles and participated in 5 research projects, some of which were supported by the Beijing Natural Science Foundation. In addition, he participates in the Youth Fund of Tsinghua University.
His current main research areas include neuro-navigation technology, multimodal image fusion, and the clinical diagnosis and treatment of spinal cord diseases.
Zhenxing Sun received the master degree from the Beijing Tiantan Hospital, Capital Medical University on July 2011 and the M.D. degree from Tsinghua University in July 2015.
Since September 2015, he has been working at the Department of Neurosurgery at the Beijing Tsinghua Changgung Hospital, School of Clinical Medicine at Tsinghua University.
He specializes in spine and spinal cord diseases, including Chiari malformation, syringomyelia, spinal cord tumors, lumbar spondylosis, and cervical spondylosis. At present, he has published 5 papers that are available in the Science Citation Index, 15 papers in core Chinese journals, and 3 bibliographic books. He has managed 2 National Natural Science Fund Projects and 1 Project from the Ministry of Health, Health Science, and Technology Development.
Dan Yuan graduated in July 2011 with the master degree from Beijing Youyi Hospital of Capital Medical University.
Since September 2011, she has been working at the Department of Nephrology at Beijing Luhe Hospital of Capital Medical University, Beijing, China. Currently, she has published 3 core Chinese journal articles and 2 Science Citation Index articles.
At present, her main research area is the clinical diagnosis and treatment of nephrological diseases.
Yaxing Sun received the bachelor degree from Taishan Medical University on July 2011. Since September 2011, he has been working at the Department of Psychiatry of Zaozhuang Mental Health Center in Shandong, China.
He specializes in mental diseases, including postoperative depression, vesania, and schizophrenia. At present, he has published 2 Science Citation Index articles and 5 core Chinese journal articles.
Zhanquan Zhang was born on May 22, 1971. In September 1991 to July 1996, he studied medicine at Lanzhou University. Currently, he works at the Department of Neurosurgery, Fifth People's Hospital in Datong City. He serves as the deputy director of the Department and is an associate professor at Datong University.
He studied micro-neurosurgery in April 2005 for one year at Tianjin Huanhu Hospital and neuro-endoscopic technology in 2011 at Qilu Hospital of Shandong University. In July 2015, he completed a spine course at Tsinghua Changgung Hospital.
Jin Wang is the deputy president and chief physician at the Department of Neurosurgery, Beijing Tsinghua Changgung Hospital, School of Clinical Medicine, Tsinghua University.
Dr. Wang acquired his USA Educational Commission for Foreign Medical Graduatescertified M.D. in 1993 and became an American Association of Neurological Surgeons-certified clinical neurosurgeon in 2003. Since 2010, Dr. Wang has been working as the chief physician at Seattle Providence Hospital and an associate professor at Washington University.
Dr. Wang has extensive experience in the surgical treatment of intracranial tumors, functional neurological diseases, and spine and spinal cord disorders. To date, Dr. Wang has published more than 30 academic articles in both domestic and foreign academic journals.
Guo Yi graduated in July 2012 from the Beijing Tiantan Hospital, Capital Medical University with the Ph.D. degree.
Since July 2015, he has been working at the Neurosurgery Department of the Beijing Tsinghua Changgung Hospital as an attending physician. Currently, he has published 7 core Chinese journal articles and 15 Science Citation Index articles and has been the principal investigator on four scientific studies.
At present, his main research areas are the clinical diagnosis and treatment of traumatic brain injury and cerebral vascular and spinal cord diseases.
Guoqin Wang graduated from Hubei Chinese Medicine University School of Nursing in June 2009.
Since August 2014, she has been working as an electrophysiologist at the Beijing Tsinghua Changgung Hospital.
Dongkang Liu graduated from Beijing Tiantan Hospital of Capital Medical University in July 2015 with the master degree.
Since September 2015, he has been a Ph.D. candidate in the Neurosurgery Department at the Beijing Tsinghua Changgung Hospital. To date, he has published 3 core Chinese journal articles and 1 Science Citation Index article.
His current main research area is the clinical diagnosis and treatment of spinal cord diseases.
Peng Cheng graduated from Beijing Union Medical College in February 2014 with the master degree.
Since March 2014, he has been working as an epidemiologist at Beijing Tsinghua Changgung Hospital.
Linkai Jing graduated in July 2016 from the Beijing Tiantan Hospital of Capital Medical University with the master degree.
Since September 2016, he has been a Ph.D. candidate in the Neurosurgery Department of the Beijing Tsinghua Changgung Hospital. His publications include 14 core Chinese journal articles and 5 Science Citation Index articles.
His current main area of research is the clinical diagnosis and treatment of spinal cord diseases.
Feng Yang graduated from Peking University in June 2014 and since has been working at the Beijing Tsinghua Changgung Hospital.
In addition, he has participated in a meta-analysis research project that was sponsored by the General Administration of Sports and in National Science Foundation-supported basic research on laser light-excitation at different wavelengths to evaluate different spectral features.
Huifang Zhang graduated from Jinlin Medical college in June 2009. From July 2009 to March 2015, she worked at Beijing Tiantan Hospital of Capital Medical University. Since then, she has been working at Beijing Tsinghua Changgung Hospital as a nurse practitioner and has recently completed the supervisor nurse examination.
Wei Shi graduated from the Medical School of the Chinese PLA in July 2015 with the Ph.D. degree.
In August 2015, he began a residency at the Neurosurgery Department of the Beijing Tsinghua Changgung Hospital. As a 3rd-year resident, he has published 1 core Chinese journal article and 2 Science Citation Index articles and participated in 4 research projects, some of which have been supported by the Beijing Natural Science Foundation.
At present, his main research areas include the clinical diagnosis and treatment of traumatic brain injury and cerebral vascular and spinal cord diseases.
Guaihuai Wang is the director and chief physician at the Department of Neurosurgery at the Beijing Tsinghua Changgung Hospital, School of Clinical Medicine at Tsinghua University.
Dr. Wang has previously mentored by renown neurosurgeon and academician Zhongcheng Wang and has more than 25 years of experience in the surgical treatment of brain stem and spinal cord tumors, spinal congenital dysplasia, and spinal degeneration diseases.
To date, Dr. Wang has performed approximately 10, 000 operations for spinal cord diseases, including a successful resection of the intramedullary tumor from the medulla oblongata to level T6, which is one of the longest reported tumors in medical history.
Thus far, he has managed 10 funded research projects and published more than 80 articles in both domestic and foreign academic journals.
Schwannomas are some of the most common spinal tumors, accounting for nearly 30% of spinal tumors[1].Intramedullary schwannomas comprise approximately 0.3% of all medullary tumors and 1.1% of spinal schwannomas[2, 3]. Schwannomas arise from Schwann cells of the neuronal myelin sheath[1-7]. There are no Schwann cells in intramedullary neural tissues; therefore, the origin of intramedullary schwannomas remains controversial. Few cases of intramedullary schwannomas have been reported since the first case was reported by Penfild et al. in 1932[4]. Intramedullary schwannomas can occur along the length of the spinal cord, including in the cervical, thoracic, or lumbar cords[2]. Magnetic resonance imaging (MRI) is an important method for diagnosing intramedullary schwannomas; however, the misdiagnosis rate remains high[3, 8, 9]. Surgical resection is the most common and effective method for treating intramedullary schwannoms[10]. In the current study, a case of intramedullary schwannoma in the cervical spinal cord is reported, along with its clinical features, radiologic and histopathologic observations, and one-year follow-up MRI results; a literature review of these aspects is also presented.
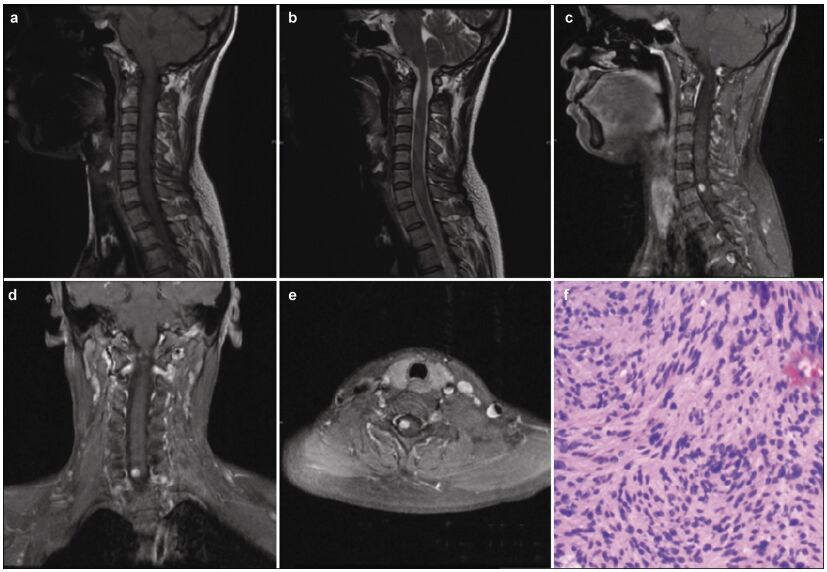
2 Case reportA 35-year-old woman presented to Beijing Tsinghua Changgung Hospital with a 10-year history of cervical malaise, which rapidly worsened over the 3 months prior to presentation. Her symptoms included right limb paraesthesia and gait deterioration due to imbalance and weakness. Her past medical and family histories did not support a neurofibromatosis diagnosis.A neurologic examination revealed grade 4 right limb muscle strength, as well as right limb pain and numbness. A right Hoffman sign (+) and exaggerated right tendon reflexes were also observed. MRI revealed an 8 mm × 6 mm × 8 mm intramedullary tumor at the C6-C7 vertebrae level. The tumor had clear margins, was isointense on T1-weighted images (Figure 1a), and was slightly hyperintense on T2-weighted images (Figure 1b). Marked homogenous contrast enhancement was also noted (Figures 1c-1e) and there were some signs of swelling around the lesion. After intraoperative O-arm navigation to determine the lesion's exact location, a small explosive incision was made in the spinal cord, between the C6 and C7 vertebrae. The tumor had clear margins and was highly adherent to the surrounding neural tissues. The tumor was completely resected using microsurgical techniques. It was a solid, soft mass, measuring approximately 8 mm × 5 mm × 2 mm. A pathological examination confirmed that the tumor was a schwannoma (Figure 1f). The patient's neurological examination improved postoperatively. One year after surgery, the patient's symptoms were in remission and a post-operative MRI revealed no evidence of tumor recurrence (Figures 2a-2d).
|
| Figure 1 (a) Sagittal T1-weighted magnetic resonance image demonstrating an isointense lesion. (b) Sagittal T2-weighted magnetic resonance image demonstrating a slightly hyperintense lesion, with swelling surrounding it. (c-e) Sagittal, coronal, and axial T1-weighted magnetic resonance images, with gadolinium contrast, demonstrating homogeneous enhancement of the tumor. The tumor appears as a solid mass, located to the right side of spinal cord, with clear margins. (f) Hematoxylin and eosin staining from the biopsy of the mass showing bipolar spindle cells with nuclei arranged in a palisade pattern (Hematoxylin & Eosin stain; magnification, ×100) |
|
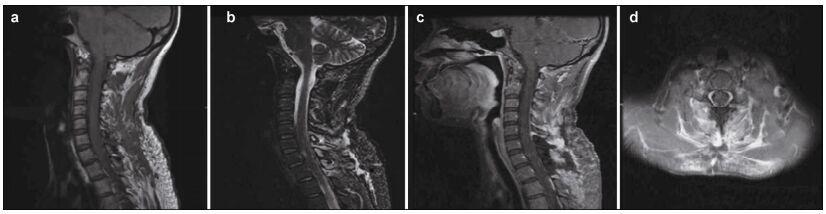
| Figure 2 Post-operative magnetic resonance image; no recurrence of the solid tumor is evident. |
Intramedullary schwannomas are very rare. Hypotheses regarding their pathogenesis include[3, 10-12]: (1) ectopic Schwann cells originating from the embryonic neural ridge; (2) Schwann cells ensheathing aberrant intramedullary nerve fibers; (3) Schwann cells extending along the branches of the anterior spinal artery; (4) neoplastic growth of Schwann cells into the cord from areas where the posterior nerve roots enter the pia mater; (5) transformation of cells with neuroectodermal origins into Schwann cells; and (6) differentiation of pulripotent mesenchysmal cells into Schwann cells. Ross et al. reviewed 22 cases of intramedullary schwannomas, and reported that the most common location of spinal intramedullary schwannomas is in the cervical cord (50%), followed by the thoracic (22%) and lumbar cords[2]. López et al. reported a 3:1 male:female ratio for the occurrence of intramedullary schwannomas[13]. The tumors are usually single lesions, most commonly in the cervical (63%), thoracic, and lumbar (11%) spinal cords[13]. The average interval between the first symptoms and a diagnosis is 28.2 months (range: 6 months to 20 years)[13]. Karatay et al. reported a case of intramedullary schwannoma located in the conus medullaris, in conjunction with syringomyelia[6].
The specific clinical manifestations of intramedullary schwannomas are associated with the tumor's size and location, but they generally exhibit the general characteristics of intramedullary tumors in that they cause upper motor neuron damage. Patients often complain of numbness, pain, paralysis, muscle atrophy, and even dyspnea. Wu et al. reported that somatic and nerve root pain are the chief complaints associated with schwannomas[14]. MRI is the most useful modality for diagnosing spinal cord tumors, but little research on intramedullary schwannomas has been reported.Our literature review indicated that schwannoma characteristics include: (1) asymmetric, solid nodules or masses, often located in the dorsolateral part of the spinal cord; (2) most lesions are small, spanning no more than three vertebral segments; (3) T1-weighted MRIs generally show an isointense or slightly hypointense lesion, T2-weighted scans show slightly hyperintense lesions, and enhanced T1-weighted scans show homogeneous enhancement, with obviously clear margins; (4) the lesions may be accompanied by cystic changes, necrosis, syringomyelia, localized swelling, and rarely, calcification[3, 6-12, 15].
Based on the articles reviewed, the most common differential diagnoses associated with intramedullary schwannomas include ependymomas, hemangioblastomas, astrocytomas, and intramedullary tuberculomas[1-7, 10-12, 14, 15]. The preoperative diagnosis of the present case was hemangioblastoma. However, the enhancement of the lesion was less obvious than that typical of a hemangioblastoma, and extensive cystic changes and vascular flow-void effects were not observed. There was also evidence of swelling, which differentiated the present lesion from a hemangioblastoma.
The goal of spinal schwannoma surgical treatment is complete tumor resection. Conti et al. reported a series of 179 patients with intramedullary tumors who were treated operatively[10]. There were three cases (1 case with neurofibromatosis) of intramedullary schwannomas, and all were totally resected and did not recur[10]. However, total removal can be difficult due to tumor adherence to the surrounding neural tissues. In these cases, subtotal removal is a wise choice for reducing postoperative complications. Since intramedullary schwannomas are benign, radiotherapy is rarely used following subtotal resection. Formal guidelines for treating recurrent tumors are lacking, but reoperation is currently the most common choice. Lee et al. reported 10 patients with intramedullary schwannomas who underwent surgical treatment and had long follow-up periods[16]. Gross total resection was performed in 8 cases, whereas subtotal resection was performed in 2[16]. The mean follow-up period was 75.7 months. The authors did not observe any cases of recurrence or clinical deterioration in these patients[15].
In conclusion, intramedullary schwannomas are very rare, but should be suspected if MRIs indicate asymmetric, solid nodules or masses, and enhanced T1-weighted scans show obvious homogeneous enhancement of the lesion, clear margins, and localized swelling. The optimal treatment is surgery, aiming for maximal resection, according to the operative situation. The patient prognosis is good, with recurrence or deterioration rarely observed.
AcknowledgementsThis project was supported by the Beijing Tsinghua Changgung Hospital Fund (No. 12015C1044). The authors thank Zhenxing Sun and Huifang Zhang for collecting the archived data and Guihuai Wang and Jin Wang for technical assistance.
Conflict of interestsNone of the contributing authors have conflicts of interest.
| [1] | Levy WJ, Latchaw J, Hahn JF, SawhnyB, Bay J, Dohn DF. Spinal neurofibromas:a report of 66 cases and a comparison with meningiomas. Neurosurgery, 1986, 18(3): 331–334. DOI:10.1227/00006123-198603000-00013 |
| [2] | Ross DA, Edwards MSB, Wilson CB. Intramedullary neurilemomas of the spinal cord:report of two cases and review ofthe literature. Neurosurgery, 1986, 19(3): 458–464. DOI:10.1227/00006123-198609000-00023 |
| [3] | Ho T, Tai KS, Fan YW, Leong LL. Intramedullary spinal schwannoma:case report and review of preoperative magnetic resonance imaging features. Asia J Surg, 2006, 29(4): 306–308. DOI:10.1016/S1015-9584(09)60108-1 |
| [4] | Penfield W. Cytology and Cellular Pathology of the Nervous System. New York: Paul B Hoeber Inc., 1932 . |
| [5] | Nicoletti GF, Passanisi M, Castana L, Albanese V. Intramedullary spinal neurinoma:case report and review of 46 cases. J Neurosurgery Sci, 1994, 38(3): 187–191. |
| [6] | Karatay M, Koktekir E, Erdem Y, Celik H, Sertbas I, Bayar MA. Intramedullary schwannoma of conus medullaris with syringomyelia. Asia J Surg, 2017, 40(3): 240–242. DOI:10.1016/j.asjsur.2014.04.004 |
| [7] | Sun B, Che XM, Gu SX, Liu XD, Shou JJ, Gu WT. The clinical diagnosis and treatment of intramedullary spinal schwannomas. Chin J Neurosurg, 2012, 28(6): 577–580. |
| [8] | Colosimo C, Cerase A, Denaro L, Maira G, Greco R. Magnetic resonance imaging of intramedullary spinal cord schwannomas. J Neurosurg, 2003, 99(1): 114–117. |
| [9] | Kodama Y, Terae S, Hida K, Chu BC, Kaneko K, Miyasaka K. Intramedullary schwannoma of the spinal cord:report of two cases. Neuroradiology, 2001, 43(7): 567–571. DOI:10.1007/s002340100540 |
| [10] | Conti P, Pansini G, Mouchaty H, Capuano C, Conti R. Spinal neurinomas:retrospective analysis and long-term outcome of 179 consecutively operated cases and review of the literature. Surg Neurol, 2004, 61(1): 34–43. DOI:10.1016/S0090-3019(03)00537-8 |
| [11] | Shenoy SN, Raja A. Cystic cervical intramedullary schwannoma with syringomyelia. Neurol India, 2005, 53(2): 224–225. DOI:10.4103/0028-3886.16419 |
| [12] | Riffaud L, Morandi X, Massengo S, Carsin-Nicol B, Heresbach N, Guegan Y. MRI of intramedullary spinal schwannomas:case report and review of the literature. Neuroradiology, 2000, 42(4): 275–279. DOI:10.1007/s002340050885 |
| [13] | López J, Diaz DR, Medina YC, et al. Schwanoma intramedular cervical. ArchNeurocien, 2004, 9: 55–58. |
| [14] | Wu L, Yao N, Chen DX, Deng XF, Xu YL. Preoperative diagnosis of intramedullary spinal schwannomas. Neurol Med Chir(Tokyo), 2011, 51(9): 630–634. DOI:10.2176/nmc.51.630 |
| [15] | Hayashi F, Sakai T, Sairyo K, HirohashiN, Higashino K, Katoh S, Yasui N. Intramedullary schwannoma with calcification of the epiconus. Spine J, 2009, 9(5): e19–e23. DOI:10.1016/j.spinee.2008.11.006 |
| [16] | Lee SE, Chung CK, Kim HJ. Intramedullary schwannomas:long-term outcomes of ten operated cases. J Neuro-Oncol, 2013, 113(1): 75–81. DOI:10.1007/s11060-013-1091-9 |



